
Health Care Costs:
Will They Start Rising Rapidly Again?
Issue Brief No. 10
June 1997
![]() ecent news reports have speculated that health care costs, which have been increasing at dramatically lower rates over the past few years, are about to take off again. But a panel convened by the Center for Studying Health System Change to discuss health care cost trends said the forces that have kept large cost increases at bay are still in effect and premium increases will be moderate. This Issue Brief reports on what the panel participants predicted is likely to happen to health care costs during the next several years and what underlying forces will shape these trends.
ecent news reports have speculated that health care costs, which have been increasing at dramatically lower rates over the past few years, are about to take off again. But a panel convened by the Center for Studying Health System Change to discuss health care cost trends said the forces that have kept large cost increases at bay are still in effect and premium increases will be moderate. This Issue Brief reports on what the panel participants predicted is likely to happen to health care costs during the next several years and what underlying forces will shape these trends.
Low-Cost Trends Continued in 1996
![]() ince 1990, the growth of health care costs has declined steadily, entering a period of historically low rates of increase beginning in 1994. This trend generally appears to have persisted through 1996, according to an index developed by the actuarial firm of Milliman & Robertson, which shows health care costs to have increased 2.0 percent during 1996, the same increase as in 1995.
ince 1990, the growth of health care costs has declined steadily, entering a period of historically low rates of increase beginning in 1994. This trend generally appears to have persisted through 1996, according to an index developed by the actuarial firm of Milliman & Robertson, which shows health care costs to have increased 2.0 percent during 1996, the same increase as in 1995.
Another striking cost trend is that private health insurance premiums rose only 0.5 percent in 1996 -- substantially below the increase in underlying costs (see Figure 1 below). It is important to differentiate between health insurance premiums and underlying health care costs. Premiums are not indicative of underlying costs. Instead, changes in underlying costs precede changes in premiums, because insurers use historical cost data to set future premium rates.
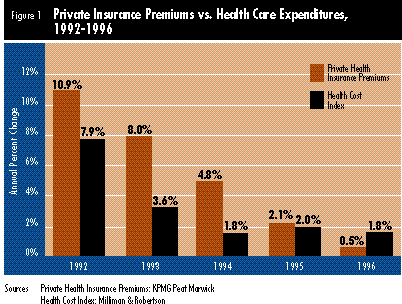
The continued decline of private health insurance premium trends to rates below cost trends probably reflects "the very new, really intense competitiveness in health insurance markets," observed Paul B. Ginsburg, president of the Center. "With employers much more willing to change health plans to get a lower premium, health care plans feel a lot more pressure from purchasers to keep their premiums down than they have ever felt before." In addition, anecdotal reports suggest that plans have been willing to restrain premium increases to build market share, Ginsburg noted.
"Obviously, this trend can’t continue forever," he added. "At some point, the health plans will have their backs to the wall." Accordingly, speculation that plans will raise their premiums by 4 percent or 5 percent in 1997 may be plausible, he said, but increases reflecting underlying cost increases around 3 percent are more likely.
It is unclear how employers would react to premium increases of this order, although they have taken several measures during the past few years to lower their health care expenditures. For example, data from the KPMG Peat Marwick survey show that employees have not benefited from premium declines to the extent that employers have (see Figure 2 below). Instead, employers have required their employees to pay a higher proportion of health insurance costs. In addition, they have changed their contribution formulas to steer their employees out of conventional insurance plans and into managed care.
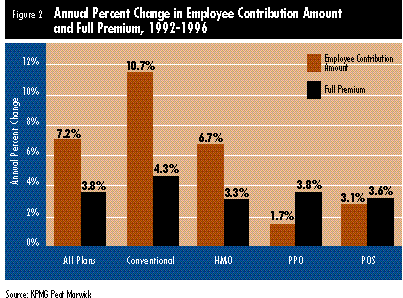
When faced with larger premium increases, employers could react by shifting even more of their costs to their employees or by protecting their employees against large increases, Ginsburg noted. Either action will attract significant attention from the media and policy makers.
The Paradigm Shift of the 1990s
![]() hat is behind these continued trends? Peter Reilly, a Milliman & Robertson actuary, suggested that the dynamics between health care consumption and general economic growth changed dramatically in 1993. Historically, he noted, health care consumption has exceeded real economic activity, meaning that the percentage of the gross domestic product spent on health care rose steadily. But that is no longer the case. "The excess growth rate has been eliminated and recently health care consumption has actually been growing below the level of where economic activity would have predicted," Reilly said. He credited the expansion and improved effectiveness of managed care with eliminating that excess growth.
hat is behind these continued trends? Peter Reilly, a Milliman & Robertson actuary, suggested that the dynamics between health care consumption and general economic growth changed dramatically in 1993. Historically, he noted, health care consumption has exceeded real economic activity, meaning that the percentage of the gross domestic product spent on health care rose steadily. But that is no longer the case. "The excess growth rate has been eliminated and recently health care consumption has actually been growing below the level of where economic activity would have predicted," Reilly said. He credited the expansion and improved effectiveness of managed care with eliminating that excess growth.
The low rate of inflation in the general economy also has helped keep health care costs in check. In addition, Medicare reimbursement to hospitals and physicians has risen significantly faster than that of other payers, resulting in favorable cost-shifting for the non-Medicare market. That cost shift will probably be eliminated this year and begin to reverse in 1998 and 1999 as a result of budgetary pressures on reimbursement levels, Reilly predicted.
It is important to note that these medical trends are proceeding against a backdrop of aggressive insurer competition and diminished insurer profitability, which started to occur in 1995 and likely will persist -- and possibly worsen -- through 1999, Reilly said. "In 1995 and 1996, insurers were spending surplus to hold on to market share that they had accumulated" during six consecutive years of profitability in the 1980s. At the same time, however, they increased their premium rates below the rate of cost growth -- "despite the fact that cost increases were at historically low levels," Reilly noted. As a result, profitability dropped to the point where insurers "were actually losing money on an underwriting basis." This loss of insurer profitability has important implications for future premium rates.
Marketplace Reinforces Cost Trends
![]() eff Goldsmith, president of Health Futures Inc., said he believes that much of the speculation regarding imminent cost increases amounts to "wishful thinking on the part of the health plans that would like the investment community to believe that they are raising their rates and that their cash flow is going to improve." Providers, too, would like people to believe that "finally they have gotten enough bargaining power to begin raising their rates and make those rate increases stick with the health plans," Goldsmith added.
eff Goldsmith, president of Health Futures Inc., said he believes that much of the speculation regarding imminent cost increases amounts to "wishful thinking on the part of the health plans that would like the investment community to believe that they are raising their rates and that their cash flow is going to improve." Providers, too, would like people to believe that "finally they have gotten enough bargaining power to begin raising their rates and make those rate increases stick with the health plans," Goldsmith added.
Expectations -- and demands -- with respect to health care costs have changed dramatically since the days of double-digit premium increases during the 1980s, and they are not likely to reverse any time soon, Goldsmith observed. He described those changed expectations as the legacy of the failed Clinton health care reform effort. In addition, the spread of managed care, and particularly the shifting of risk from payers to providers, has heightened providers’ incentives to restrain costs, Goldsmith said. As a result, private-sector purchasers, who for years had little choice but to accept large increases in their health care expenditures, have come to expect lower costs. They have been pressuring insurers and providers to keep costs under control, and the purchasers’ success has lent credence to those expectations. There is no reason to believe that employers will ease those demands.
The landscape of the U.S. health care delivery system has changed significantly in other ways as well, Goldsmith said. Instead of the managed competition system prophesied by the Jackson Hole Group and other managed care advocates, the failure of federal health reform led to the expansion of managed care in an environment of "unmanaged competition," where "policy makers are free to parachute in and declare entitlements to particular services" without comprehensive regulation of health insurance provision, which continues to be a state prerogative.
|
||
Despite the absence of comprehensive health reform, market forces have compelled insurers to respond to employers’ and consumers’ demands for lower prices and greater provider choice. "It has taken a while for that message to ripple back through the health insurance system," Goldsmith noted.
Employers seeking to leverage their purchasing power and consolidate vendors have decided to narrow their employees’ choices of insurance carriers. According to Goldsmith, 50 percent to 70 percent of all employers offer their employees only one insurance carrier. But that single carrier has been forced to accommodate consumer demands for greater choice by offering multiple products -- including HMO, PPO and POS plans -- with broad, overlapping networks that include virtually all the providers in the local marketplace.
What About the Future?
![]() t is unclear how this phenomenon of continued price constraint and network inclusiveness will play out ultimately, but in mature managed care markets, such as Portland, Ore., and Los Angeles, it has caused a crisis of differentiation among health plans. In these markets, price competition has become so intense that there is now very little difference in price between the most expensive and the least expensive plan. And because all the plans include virtually the same providers in their networks, they now find themselves at a loss about how to compete convincingly with each other. "The basis for differentiating the plans from one another is moving into an area where no one really knows exactly what to do," Goldsmith said.
t is unclear how this phenomenon of continued price constraint and network inclusiveness will play out ultimately, but in mature managed care markets, such as Portland, Ore., and Los Angeles, it has caused a crisis of differentiation among health plans. In these markets, price competition has become so intense that there is now very little difference in price between the most expensive and the least expensive plan. And because all the plans include virtually the same providers in their networks, they now find themselves at a loss about how to compete convincingly with each other. "The basis for differentiating the plans from one another is moving into an area where no one really knows exactly what to do," Goldsmith said.
In addition, the emergence of these sprawling, inclusive networks carries important cost implications. During the early years of managed care growth, providers, fearing exclusion from health plan networks and loss of income, acceded to plans’ demands for large price discounts. "When providers realize that the threat to exclude them from networks is less credible with each passing year, it may be difficult for health insurers to continue getting that level of panic-driven discounts," Goldsmith observed. That does not mean, however, that private-sector health care costs will spiral again.
|
||
First, most major markets continue to experience excess capacity of hospitals and specialists. "In many major metropolitan areas, we still have half again the number of hospitals, the amount of hospital capacity, the number of operating suites and the number of gastroenterologists that we need to service the population," Goldsmith observed. Provider supply, then, remains unchanged -- leaving providers, in Goldsmith’s opinion, with insufficient economic leverage to raise their prices for health plans "enough to reignite health-cost inflation on the private side."
Second, the influx of Medicare and Medicaid enrollees into managed care is increasing health plans’ clout over providers, especially with respect to Medicare, which accounts for more than 40 percent of a typical hospital’s revenues and 60 percent of specialists’ revenues. That leverage gained by plans through increased Medicare enrollment ultimately benefits private purchasers as well, Goldsmith noted.
In the long term, Goldsmith said he foresees tremendous savings opportunities as managed care organizations become more sophisticated in their efforts to control costs. Looking even farther ahead, he added, those opportunities will take on new dimensions should Medicare depart from its cost-based method of paying health plans and put health plan premiums up for bid. Such a move undoubtedly would send plans in some localities reeling from the impact on their revenues, but it also would finally set in motion the forces needed to remove excess provider capacity from the delivery system.
|
||
The panelists concluded that the forces that have kept health care costs in check during the past few years will remain in effect for the most part. While those forces may not hold trends for costs and premiums to their current historic lows, they will moderate increases for the next several years. Reilly projected that by the end of 1997, cost increases underlying private insurance will climb from about 2 percent to 4 percent or perhaps as much 5 percent, rising slightly in 1998 and then leveling off again in 1999. This forecast assumes an underlying general inflation rate of 3 percent. It also assumes that the excess growth rate between health care costs and general economic activity remains eliminated. It is important to note that costs likely will vary across local markets, depending on such factors as the level of managed care and provider strength.