
Relief, Restoration and Reform: Economic Upturn Yields Modest and Uneven Health Returns
Issue Brief No. 117
January 2008
Robert E. Hurley, Aaron Katz, Laurie E. Felland
The sensitivity of state budgets to economic cycles contributes to fluctuations in health coverage, eligibility, benefits and provider payment levels in public programs, as well as support for safety net hospitals and community health centers (CHCs). The aftershocks of the 2001 recession on state budgets were felt well into 2004. More recently, the economic recovery allowed many states to restore cuts and, in some cases, expand health services for low-income people, according to findings from the Center for Studying Health System Change’s (HSC) 2007 site visits to 12 nationally representative metropolitan communities. Along with bolstering support of safety net providers and raising Medicaid payments for private physicians, some states advanced even more ambitious health reform proposals. Yet across communities, safety net systems face mounting challenges of caring for more uninsured patients, and these pressures will likely increase given the current economic downturn.
- State Budget Cycles Hinder Stability for Safety Net Providers
- Relief: Economic Recovery
- Restoration: Rollback of Cuts
- Reform: Ideas and Realities
- Future Expectations and Anxieties
- Notes
- Data Source
State Budget Cycles Hinder Stability for Safety Net Providers
![]() rowing concerns about an economic downturn underscore the
degree to which public support for services for low-income people is dependent
on larger economic forces. HSC site visits from the early to mid-2000s reported
extensively on the consequences of the 2001 recession (see Data
Source). As more people became eligible for public insurance or lost private
coverage, primarily because of growing unemployment, enrollment in Medicaid
and the State Children’s Health Insurance Program (SCHIP) increased significantly,
and safety net providers appeared more beleaguered.
rowing concerns about an economic downturn underscore the
degree to which public support for services for low-income people is dependent
on larger economic forces. HSC site visits from the early to mid-2000s reported
extensively on the consequences of the 2001 recession (see Data
Source). As more people became eligible for public insurance or lost private
coverage, primarily because of growing unemployment, enrollment in Medicaid
and the State Children’s Health Insurance Program (SCHIP) increased significantly,
and safety net providers appeared more beleaguered.
With a few exceptions, state and local policy makers—to balance their budgets as required by law—had to make difficult cuts in public program coverage, provider payments and key service areas like mental health and public health. Even though the federal government provided a temporary $10 billion increase in Medicaid matching funds in 2003 and 2004, declines in federal support for other human service programs and relatively stagnant grant funding to existing community health centers added to the distress. Some states put planned Medicaid expansions on hold, while others cut Medicaid eligibility and provider payments to help meet balanced-budget obligations, responding to the fact that Medicaid accounts for more than 20 percent of total state spending.1 All of these factors intensified pressures on providers that are less able to turn away Medicaid and uninsured patients because of their mission or proximity to low-income neighborhoods at the same time these providers faced sharply rising operating expenses.
The 2007 site visits revealed a more upbeat picture in most states—improved tax collections, increased provider revenues from Medicaid and SCHIP, and a healthier employment climate. With this relief, restoration was the order of the day, and some states pursued coverage expansions and other reforms, contributing to a stable, if not stronger, financial condition for most safety net providers. While this “rolling recovery” had exceptions, the past half-decade illustrates how larger economic conditions powerfully affect what communities can be expected to achieve and sustain related to health care for low-income people.
Back to Top
Relief: Economic Recovery
![]() hile the 2001 recession had the most severe impact on state
revenues since World War II, recovery was rapid and robust in most states, and
a turnaround in state tax collections was broadly evident beginning in 2004
(see Figure 1). The brightened economic picture was apparent
as unemployment began to fall, enrollment in the Medicaid program slowed (and
declined in 2007 for the first time in the past decade) and overall Medicaid
cost trends moderated. As one Seattle policy maker said, “The tide has turned,
so instead of cuts, we’ve seen some modest additions; we’re not where we were,
but we’re heading back.”
hile the 2001 recession had the most severe impact on state
revenues since World War II, recovery was rapid and robust in most states, and
a turnaround in state tax collections was broadly evident beginning in 2004
(see Figure 1). The brightened economic picture was apparent
as unemployment began to fall, enrollment in the Medicaid program slowed (and
declined in 2007 for the first time in the past decade) and overall Medicaid
cost trends moderated. As one Seattle policy maker said, “The tide has turned,
so instead of cuts, we’ve seen some modest additions; we’re not where we were,
but we’re heading back.”
The recession-to-relief turnaround reveals an underlying volatility of state budgets, which is associated with many factors, including local economic conditions, sources of tax revenues, changes in spending priorities, magnitude of reserve funds, and policy decisions to limit tax increases and reduce spending. Nonetheless, some states like Arkansas and Arizona were spared much of the turbulence because of diversified economies, and only Michigan—the victim of a so-called “one-state recession”—and New Jersey failed to see a sizable fiscal improvement in the past two years.
State budget and economic instability also plays a major role in public financing of health programs and safety net providers. In communities like Miami, Indianapolis, Cleveland and Phoenix, local property tax levies are critical sources of support for safety net hospitals, while safety net hospitals in Boston and northern New Jersey receive substantial financial support from charity care pools funded in part with state taxes. Federal Medicaid disproportionate share hospital (DSH) funds that help finance care for uninsured people have been a longstanding element of funding in nearly all of the communities, with Boston, Miami and Orange County particularly reliant on DSH funds. Programs to reimburse providers for services for uninsured people in Indianapolis and Lansing have directed additional dollars to providers that treat the uninsured. Through the economic decline and recovery, however, the funding generated by these mechanisms has fluctuated, in part because of federal policy changes.
Partially because of the cyclical nature of state revenues and Medicaid spending, state and local policy makers have pursued new funding sources in recent years to provide additional support to community safety net providers. For example, Proposition 63 in California earmarked new state taxes for mental health services; the Children’s Trust property tax levy in Miami raises funds for health and human services for children; and a new special taxing authority provides financial support for the county health system in Phoenix.
Long-awaited federal funds for emergency care of undocumented immigrants have provided a modest infusion of funding for hospitals in a few of the 12 communities. Some communities like northern New Jersey and Orange County benefited from additional federal funding for new community health centers. A sharply increased cigarette tax in Indiana provided additional revenue to fund health initiatives, and in several communities, including Miami and Orange County, rapid increases in housing prices generated property tax windfalls that local officials used to bolster funding for safety net providers.
“We’re riding fat budgets due to the housing market,” one Florida policy maker noted in spring 2007.
Back to Top
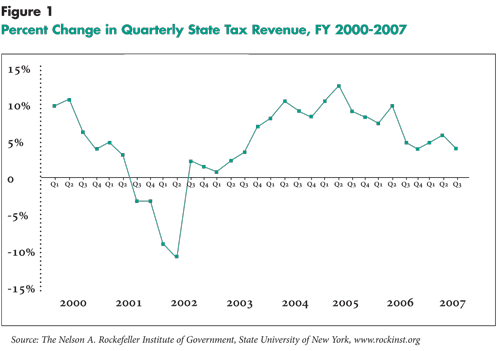 |
Click here to view this figure as a PowerPoint slide.
Restoration: Rollback of Cuts
![]() here did policy makers place their priorities as they made the most of this improving economic picture and what have been the consequences for low-income people and safety net providers?
here did policy makers place their priorities as they made the most of this improving economic picture and what have been the consequences for low-income people and safety net providers?
Enrollment in Public Programs. In most markets, restoration has focused on reversing earlier reductions in Medicaid eligibility criteria, such as for adults in Cleveland and immigrant children in Seattle, or reverting to 12-month guaranteed periods of eligibility after shortening them to trim program participation, as in Seattle and Syracuse. Enrollment ceilings and wait lists imposed on state-sponsored, non-Medicaid coverage programs like the Basic Health Plan in Seattle and child health programs in Lansing and Miami were eased or lifted. SCHIP outreach efforts were intensified and expanded in Syracuse, Orange County, Cleveland and Miami as momentum for growth was reignited, and several states explored increasing children’s income eligibility limits for SCHIP.
Benefits, Service and Provider Payments. States also have tried to repair some of the damage from benefit cuts or limits placed on services during the aftershocks of the recession. Recovering lost funding in mental health and public health was a major priority in Boston. Other states have focused on restoring and enhancing provider payments. The New Jersey Legislature committed state funds to sharply increase Medicaid payment rates for pediatric care, which have been among the lowest in the nation. In Indiana, a 44-cent increase in the state cigarette tax enabled the state to increase Medicaid provider payments. Orange County benefited from a long-awaited improvement in state payment rates to CalOptima, the capitated local authority that operates the county’s Medi-Cal (Medicaid) program, which had experienced a prolonged period without rate increases. Orange County’s real estate tax windfall also allowed the county to pump additional funds into a local program that pays providers for services to medically indigent residents.
Exceptions to these trends were noted in Lansing where—in the interest of attempting to sustain eligibility for Michigan’s public coverage programs—a physician fee cut of 6 percent was proposed on top of a previous 4-percent rate cut, further raising concerns about access to care for Medicaid patients, especially for specialty services. Medicaid enrollment has continued to expand because of the weakening economy, though the state has frozen enrollment in a limited-benefit program for low-income adults.
The net effect of these state efforts has been to bolster support for safety net providers, including both hospitals and community health centers, in most communities and, at least in some markets, also for physicians in private practice. Eligibility restorations and expansions have converted some uninsured persons to covered status; safety net hospitals in particular have benefited from these coverage expansions for low-income adults who receive care in emergency departments or inpatient units. In nearly every community, including even Lansing, the revenue picture for community health centers has improved, though generally not fast enough to keep up with growing demand.
Yet some services have not particularly benefited from the improved budget situation. For example, mental health funding has not been restored or enhanced across the 12 HSC communities—California’s Proposition 63 is an important exception—and in the view of many observers, the availability of mental health care continues to deteriorate. Safety net hospital emergency departments and CHCs reported treating more Medicaid and uninsured patients with mental health conditions who lack other, more appropriate treatment options. Inpatient mental health capacity remains in short supply across the 12 communities, with some safety net hospitals hesitant to add capacity in this area because of insufficient payment.
Back to Top
Reform: Ideas and Realities
![]() ne of the most notable features of states’ improved financial
positions was widespread resurrection of interest in health care reform, typically
focused on coverage expansion. In this regard, Massachusetts clearly led the
way with its aim for near-universal coverage. The Massachusetts plan, enacted
in 2006, is using charity care funds to instead subsidize insurance coverage
for uninsured people. That provision, along with expansions of public insurance
programs, restructuring of insurance markets, and an individual health insurance
mandate, is intended to move the state toward universal coverage.2
The governor of California also unveiled an ambitious reform plan but has been
unable to build political consensus for the proposal.
ne of the most notable features of states’ improved financial
positions was widespread resurrection of interest in health care reform, typically
focused on coverage expansion. In this regard, Massachusetts clearly led the
way with its aim for near-universal coverage. The Massachusetts plan, enacted
in 2006, is using charity care funds to instead subsidize insurance coverage
for uninsured people. That provision, along with expansions of public insurance
programs, restructuring of insurance markets, and an individual health insurance
mandate, is intended to move the state toward universal coverage.2
The governor of California also unveiled an ambitious reform plan but has been
unable to build political consensus for the proposal.
The reform strategies introduced in Washington, Indiana and Arkansas were more limited and did not include specific provisions to attain universal or near-universal coverage. Other states like New Jersey, New York and Arizona avoided new initiatives and opted instead to try to maintain or expand coverage via existing public programs, such as SCHIP. These too face uncertain success either because of in-state political opposition, as seen in Arizona, or resistance from federal officials, in the cases of New York and New Jersey.3 Other states have followed reform developments with interest but caution.
With the economy now slowing, some state policy makers and advocates continue to voice enthusiasm for reform efforts. But the fiscal and political realities in most states limit the scope of these efforts, which seem unlikely to make a major difference in the coverage picture. In the few states pushing broader reforms, the models being advanced place safety net providers in a difficult position—wanting to support aggressive initiatives toward universal coverage, while also worrying that even if the reforms largely succeed they will be left to care for people and services that remain uncovered, such as mental health.
Back to Top
Future Expectations and Anxieties
![]() iven the cyclical nature of state revenue trends, states already are bracing for a reversal of fortune. The anticipated waning of state revenues resulting from an economic slowdown is accelerated in states where elected officials have curtailed revenue growth with either tax and spending limits, like those in Ohio, or rolled back sales taxes, such as on groceries in Arkansas.
iven the cyclical nature of state revenue trends, states already are bracing for a reversal of fortune. The anticipated waning of state revenues resulting from an economic slowdown is accelerated in states where elected officials have curtailed revenue growth with either tax and spending limits, like those in Ohio, or rolled back sales taxes, such as on groceries in Arkansas.
Because of the imprecision of state revenue forecasts, lawmakers struggle with the timing of these kinds of adjustments and not uncommonly trigger self-inflicted shortfalls in subsequent years. Moreover, earmarked funding sources—such as the tobacco settlement—can be difficult to sustain in the face of competing needs and declining revenues. Declines in cigarette tax revenues because of reduced smoking rates also are affecting some states, though some have countered this effect by further increasing tax rates. Concern is already growing in Massachusetts that tax revenues are not rising fast enough to maintain subsidies to make mandated coverage affordable for low-income residents, as well as sustaining the state’s Medicaid program.4
The decline in housing prices—after a dramatic increase in recent years—presents new threats to communities and the services they support with property tax levies, such as health care facilities and programs for low-income persons. Growth-oriented areas like Miami and Phoenix will see the effects of an economic slowdown magnified by the housing slump and home mortgage problems. Markets with disproportionate numbers of mortgage defaults, like Cleveland, will see more demand for care from safety net providers as property tax revenues fall.
As part of an economic stimulus package to head off a recession, Congress is considering another temporary increase in federal matching funds for state Medicaid programs. As past evidence shows, however, the impact on care for low-income people would likely vary across states, depending on whether states use the funds to prevent Medicaid cuts or expand Medicaid coverage.
Regardless of whether Congress approves a temporary Medicaid increase, Medicaid financing will remain a pressing concern in many states because an economic slowdown will place greater demands on the system. Moreover, the Miami, Boston and Orange County markets have been or will be deeply affected by the outcomes of high-stakes waiver negotiations between state and federal Medicaid officials, particularly related to restructuring uncompensated care programs to cover more people and provide fewer direct subsidies to providers.5 More broadly, state worries are compounded by the increased federal scrutiny of how states draw down federal dollars to finance and operate their Medicaid programs—mechanisms that have helped states during challenging economic periods. Keen federal interest in curbing growth in DSH payments and imposing more demanding conditions for documenting state Medicaid matching funds is having a palpable effect on state decision makers.
On top of this has been the angst about SCHIP reauthorization, which looked to be highly likely at the beginning of the site visits (February) but became more uncertain by the end of the visits (June). In light of the temporary reauthorization to March 2009, questions about the future design and financing of SCHIP remain additional sources of uncertainty weighing on states and the providers and enrollees in the program.6 Taken together, wavering state financial wherewithal and the turbulent nature of Medicaid and SCHIP program financing represent a sober, albeit familiar, message to the provider community that has traditionally served low-income, uninsured and Medicaid patients.
The resolution of each of these critical issues will impact the financial well being of safety net hospitals and community health centers in the 12 communities. Heavy reliance on state and local support ensures some comfort, as well as considerable uncertainty that rises and falls with state and local budgets. It also means that bold, expansive reform initiatives are difficult to launch and even more difficult to sustain in the face of economic cycles. As the latest rendition of a particularly robust recovery cycle with limited gains in major state health reform runs its course, advocates of the virtues of states as laboratories of health reform are likely to face increased skepticism.
Back to Top
Notes
| 1. | The Fiscal Survey of States, National Governors Association, National
Association of State Budget Officers (December 2007). |
| 2. | Felland, Laurie E., Debra A. Draper and Allison Liebhaber, Massachusetts
Health Reform: Employers, Lower-Wage Workers and Universal Coverage,
Issue Brief
No. 113, Center for Studying Health System Change, Washington, D.C.
(July 2007). |
| 3. | Kershaw, Sarah, “8 States to Press Bush on Health Bill,” The
New York Times, (Oct. 2, 2007). |
| 4. | Dembner, Alice, “Success Could Put Health Plan in Red,” The Boston Globe, (Nov. 18, 2007). |
| 5. | Medicaid Hospital Waivers, California HealthCare Foundation (April 2006). |
| 6. | “President Bush Signs SCHIP Extension, Provides Funds Through March 2009,” Kaiser Daily Health Policy Report (Jan. 2, 2008). |
Back to Top
Data Source
Approximately every two years, HSC conducts site visits to 12 nationally representative metropolitan communities as part of the Community Tracking Study to interview health care leaders about the local health care market, how it has changed and the effect of those changes on people. The communities are Boston; Cleveland; Greenville, S.C.; Indianapolis; Lansing, Mich.; Little Rock, Ark.; Miami; northern New Jersey; Orange County, Calif.; Phoenix; Seattle; and Syracuse, N.Y. The sixth round of site visits was conducted between February and June 2007 with more than 500 interviews. This Issue Brief is based primarily on responses from state and local policy makers, community health center and safety net hospital executives, and consumer advocates.
Back to Top
ISSUE BRIEFS are published by the
Center for Studying Health System Change.
600 Maryland Avenue, SW, Suite 550
Washington, DC 20024-2512
Tel: (202) 484-5261
Fax: (202) 484-9258
www.hschange.org