A Primer on Understanding Health Care Cost Trends:
The Story Behind the Numbers
Issue Brief No. 05
December 1996
![]() irtually every study shows that rates of increase in health care costs have declined throughout the 1990s, but often the bottom-line numbers differ. There are numerous reasons for this disparity, including which data are used and how researchers analyze them. Unfortunately, there is no ideal source of data; the best sources vary widely with regard to accuracy, timeliness, and, most important, whether the information lines up with the questions that are being asked. This Issue Brief provides information about how to understand what the numbers really represent.
irtually every study shows that rates of increase in health care costs have declined throughout the 1990s, but often the bottom-line numbers differ. There are numerous reasons for this disparity, including which data are used and how researchers analyze them. Unfortunately, there is no ideal source of data; the best sources vary widely with regard to accuracy, timeliness, and, most important, whether the information lines up with the questions that are being asked. This Issue Brief provides information about how to understand what the numbers really represent.
What Is Being Measured?
![]() hen a government or employer survey reports that the rise in health care costs is slowing, the first questions to ask are: What is the study measuring? All health care costs? Whose health care costs? It is important to know this because in almost all cases the data presented in the study have been prepared and adjusted to answer a particular policy or research question.
hen a government or employer survey reports that the rise in health care costs is slowing, the first questions to ask are: What is the study measuring? All health care costs? Whose health care costs? It is important to know this because in almost all cases the data presented in the study have been prepared and adjusted to answer a particular policy or research question.
For example, when analyzing Medicare data to measure progress in controlling costs, researchers often adjust for general inflation and changes in the population served. This is done to separate out changes that result from factors other than cost control efforts, such as the aging of the population. However, if researchers want data to plan financing for Medicare in the 21st century, demographic trends would be critical and, accordingly, they would not want to adjust for them.
Another way to look at health care data is by the various components -- for example, the amount spent for hospital care, on physicians, and for drugs. These data can show important trends in the quantity and price of services. They also can provide insight into what is behind the overall trends in health care costs and a basis for projecting future cost trends.
Employer surveys use premium costs as a proxy for health care costs. Most employer surveys gather data on the total premium cost -- that is, both the employers’ and employees’ share. Trends in premium costs are a rich source of information for employers, but are often a poor indicator of health care cost trends.
How Data Vary by Source
![]() he three major types of data used to develop cost trends are provider costs, claims incurred by insurers, and premiums paid by employers. Data ideally should be timely, cover the entire population, reflect resources used in providing services rather than what is paid for them, and provide insight into the performance of different types of health plans. In reality, each of the major sources of health data has its strengths and weaknesses.
he three major types of data used to develop cost trends are provider costs, claims incurred by insurers, and premiums paid by employers. Data ideally should be timely, cover the entire population, reflect resources used in providing services rather than what is paid for them, and provide insight into the performance of different types of health plans. In reality, each of the major sources of health data has its strengths and weaknesses.
Cost data from providers score well in a number of dimensions. They are the most timely, in large part because providers log cost or expense information as it happens. They also cover the entire population, including the uninsured. A weakness of cost data is that hospitals are the main source of information, and there is a paucity of good data available from other providers, such as those operating home health services and clinical laboratories. This problem is likely to increase over time as inpatient services continue to decline as a percentage of health care spending.
Claims data from insurers provide complete spending information for covered services. Moreover, the data not only can show expenditures but also can separate them into price and quantity components. Because of the proprietary nature of the information, however, it is not possible to get claims data from all insurers. In addition, health maintenance organizations (HMOs) record visits by encounters not claims (if they record them at all), and encounter data generally cannot be combined with claims data. This means that claims data provide an indicator of cost trends only for a nonrepresentative and declining segment of the health care system. Another weakness of claims data is that changes in the benefit structure are difficult to capture.
|
||
Premium data from employers let researchers track trends by type of health plan. This is useful for learning about the mechanisms behind changes in cost trends. For example, are changes due to a shift in enrollment from fee-for-service plans to HMOs? Are both types of health plans experiencing a slowing of the increase in premium?
On the downside, premium data are not as timely as they appear. Premiums are established months in advance based on claims data, and generally are in effect for a year. For example, 1996 premiums may have been set in late summer 1995 based on experience since the beginning of that year. Premiums also reflect a three-year underwriting cycle in which premiums play catch up based on real claims experience. If they were set too high, premiums might remain the same for two years; if they had been set too low, premiums might rise steeply. In other words, the current premium is not likely to reflect the current underlying claim costs.
Other drawbacks of premium data are that employer data exclude people covered by Medicare and Medicaid and the uninsured and, therefore, are not representative of the nation. In addition, as with insurer data, they do not separate out the effects of any changes in the benefit structure.
|
||
A Matter of Interpretation
![]() he limitations in health care cost data are compounded by people who use them for purposes other than the ones they are intended for. For example, employer surveys are not designed to track cost trends in the economy. Instead, they are designed to let employers know what they are spending on health insurance and what benefits they are giving their employees, especially compared with other employers. They are a tool for competition in the business place, not a measure of trends in health care expenditures or of how well the nation has been able to control health care costs.
he limitations in health care cost data are compounded by people who use them for purposes other than the ones they are intended for. For example, employer surveys are not designed to track cost trends in the economy. Instead, they are designed to let employers know what they are spending on health insurance and what benefits they are giving their employees, especially compared with other employers. They are a tool for competition in the business place, not a measure of trends in health care expenditures or of how well the nation has been able to control health care costs.
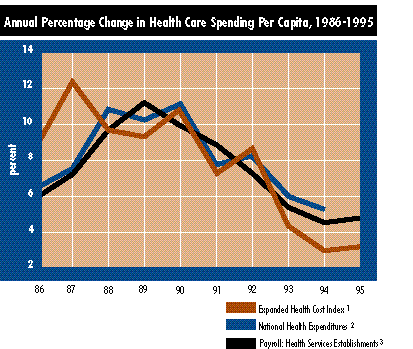
1. Calculations using data from Milliman & Robertson’s Health Insurance Trend Model and expanded to include Medicare.2. From the Health Care Financing Administration, National Cost Estimates Unit. Reflects revisions published in May 1996.
3. From the Bureau of Labor Statistics, Employment, Hours, and Earning. Payroll calculated as the product of production workers, average hours per week, and average hourly wage.
|
|
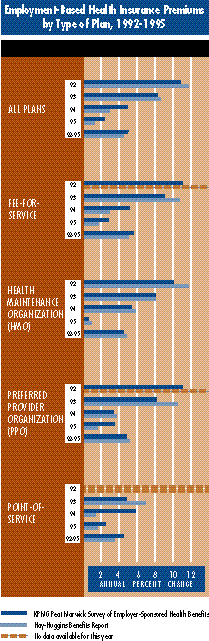
While generically the same, the employer surveys differ for a number of reasons, including the samples used. For example, both employer surveys referenced here show a significant decline in premium costs for all kinds of plans -- fee-for-service as well as managed care -- but the numbers are not the same. KPMG Peat Marwick and Hay-Huggins not only have different firms in their samples, they also have different methods of drawing their samples. The Peat Marwick survey is a stratified random sample; Hay-Huggins’s is drawn from its clients with some additional firms to make it representative. There are other differences when changes in benefit structure are considered. Actuaries at Hay-Huggins, for example, performed an analysis for the Center for Studying Health System Change that looked at changes in benefit structure by plan type from 1993 to 1995. They found the benefit structure of fee-for-service plans virtually unchanged, while the benefits in the average HMO had increased somewhat. The data behind the graph do not incorporate this actuarial analysis. When benefits are adjusted for, HMO premium increases are between 0.5 and 1.0 percent lower per year. |
Survey results also can differ by the way the change in premium is calculated. For example, another employer survey, which showed a lower rate of increase, based its calculations on the average premium across all plans. But since people are switching from traditional plans to managed care plans, which tend to have lower premiums, the trend in the average premium will be lower than a weighted average of the trends for each type of plan. The extent to which lower cost trends come from shifts among plan types versus by plan type has implications for the way people perceive the future of health care costs. For example, the cost outlook is more encouraging if each plan type is slowing its rate of premium increase, rather than if premiums are growing just as fast as before but more people are switching to plan types with lower premiums.
Reading Behind the Headline
![]() he headline of a recent release of data from the Department of Labor (DOL) reads: "Growth in employers’ health costs slows." Does this mean that cost controls are really working? The data behind the story are based on the Employment Cost Index, which includes a component for health insurance costs borne by employers.
he headline of a recent release of data from the Department of Labor (DOL) reads: "Growth in employers’ health costs slows." Does this mean that cost controls are really working? The data behind the story are based on the Employment Cost Index, which includes a component for health insurance costs borne by employers.
|
||
Several reasons are cited for the slowing growth in employer health insurance costs, but many of them have little to do with overall efforts to control costs. Rather, they reflect:
- shifting costs from employers to employees -- e.g., employees pay a greater share of the premium; and
- a drop in the proportion of employees receiving employer-sponsored health insurance either because the employer stopped offering it or because the employees -- usually people in low-paying jobs -- are less likely to enroll, especially for dependent coverage.
|
||