
CHIPing Away at the Problem of Uninsured Children
Issue Brief No. 14
August 1998
James D. Reschovsky, Peter J. Cunningham
The State Children’s Health Insurance Program (CHIP), enacted one year ago this August, is the largest expansion of health insurance in more than three decades. One of the measures of its success will be whether state officials are able to enroll children who are eligible. Research conducted by Health System Change (HSC) shows that uninsured children are a diverse group, and that for CHIP to be successful, policy makers will need to target programs to specific groups and local market conditions. This Issue Brief discusses why children lack health insurance and the implications for implementing CHIP.
The Scope of CHIP
![]() nder CHIP, created by the Balanced Budget Act of 1997, block grants are available to states to expand Medicaid eligibility for children, establish a new program that subsidizes private insurance for children or combine the two1. Congress authorized $40 billion over the next 10 years to help pay for CHIP. All states and the District of Columbia, with the exception of Washington and Wyoming, have developed or are in the process of developing a CHIP implementation plan.
nder CHIP, created by the Balanced Budget Act of 1997, block grants are available to states to expand Medicaid eligibility for children, establish a new program that subsidizes private insurance for children or combine the two1. Congress authorized $40 billion over the next 10 years to help pay for CHIP. All states and the District of Columbia, with the exception of Washington and Wyoming, have developed or are in the process of developing a CHIP implementation plan.
States have considerable latitude in designing their programs: 20 are expanding Medicaid, 14 are developing new programs that subsidize private insurance and 15 are combining the two approaches. Most of the states that combine the two approaches are relying largely on new programs, expanding Medicaid only to cover specific subgroups. HSC research, based on the latest available information at press time, indicates that 33 percent of all uninsured children will be newly eligible under CHIP expansions.
The ultimate success of CHIP -- how many uninsured, eligible children obtain coverage -- does not depend primarily on whether states pursue public or private insurance options, but rather on program implementation. It is clear from HSC findings that states need to understand the specifics of why children are uninsured before they can design and implement CHIP effectively. Although uninsured children represent a diverse group, they are largely children of the working poor. Four-fifths of the children have parents who work, yet nearly 80 percent of the children live in families with incomes below 200 percent of poverty, according to the HSC’s Household Survey. (See end of page for a discussion of the survey methodology.)
Why Children are Uninsured
![]() ost children in the United States get health insurance coverage through a parent’s employer-sponsored plan; some obtain coverage through public programs. The major reasons children go without insurance are:
ost children in the United States get health insurance coverage through a parent’s employer-sponsored plan; some obtain coverage through public programs. The major reasons children go without insurance are:
- their parents lack access to employer-sponsored health insurance;
- their parents choose not to enroll them in the plan offered by their employer;
- there are gaps in eligibility for public insurance; or
- parents fail to enroll their eligible children in publicly financed insurance programs.
Limited Access to Employment-Based Plans
The single most important reason children are uninsured -- affecting three out of four children -- is that their parents lack access to employer-sponsored health insurance because their parents are unemployed, their employers do not offer health benefits or they are ineligible for the plan that is offered. (See pie chart.) Among these reasons, employers not offering health benefits is the most important, affecting two in five uninsured children. One in five uninsured children do not have a working parent in the home. Fifteen percent of parents are not eligible for their employer’s plan, either because they have not worked for the firm long enough, or they do not work (or are not offered) enough hours to qualify for insurance.
Parents Decline Coverage for Children
Another reason children are uninsured is that their parents are offered but decline to participate in an employer-sponsored health insurance plan. This is the case for 9 percent of uninsured children. The overwhelming reason for doing so -- cited by 84 percent of respondents -- is the cost of premiums, deductibles, copayments and uncovered services. Only 12 percent of respondents said they did not need or want the insurance.
Some parents opted for health insurance for themselves, but did not extend it to their child or children. This is the case for 15 percent of all uninsured children. Two possible reasons may be that the firms did not offer family coverage or the parents declined to enroll in family coverage because it involved additional costs. The latter reason is most likely, since 98 percent of employees are in firms that offer dependent coverage. (See HSC Data Bulletin to be published in September.) Moreover, employers often do not subsidize family coverage to the extent they do employee-only coverage, which suggests that parents do not enroll their children due to the extra cost.
Gaps in the Coverage of Public Insurance
About 5.7 million children, or 65 percent of all uninsured children, were not eligible for Medicaid when Congress enacted CHIP. The new program will help fill the gaps somewhat, but 31 percent of all uninsured children -- some 2.7 million -- will remain ineligible for federally supported health insurance.
Failure to Enroll Eligible Children
Prior to the enactment of CHIP, more than one-third of uninsured children, totaling 3.1 million, were eligible for Medicaid but were not enrolled. These children constituted about 16 percent of all Medicaid-eligible children. Parents may be unaware of their children’s eligibility, may not perceive the need for insurance or may not choose to enroll them because of the stigma associated with Medicaid. In addition, there are hassles involved in determining eligibility and enrolling, as well as language barriers and other obstacles. Recent changes may exacerbate this eligibility problem. Historically, most children eligible for Medicaid were enrolled when parents signed up for welfare. But with expanded public insurance eligibility among children and changes in welfare laws, states will need to look beyond the welfare office to find children eligible for Medicaid and other public health insurance programs.
Variation Across Communities
![]() lthough the problem of uninsured children is often thought of as national, its scope and nature vary tremendously at the local level. In HSC’s 12 study sites, there is a fivefold difference between uninsurance rates for children in Lansing, the site with the lowest rate -- 4.4, and Miami, the site with the highest rate -- 22.4 percent.
lthough the problem of uninsured children is often thought of as national, its scope and nature vary tremendously at the local level. In HSC’s 12 study sites, there is a fivefold difference between uninsurance rates for children in Lansing, the site with the lowest rate -- 4.4, and Miami, the site with the highest rate -- 22.4 percent.
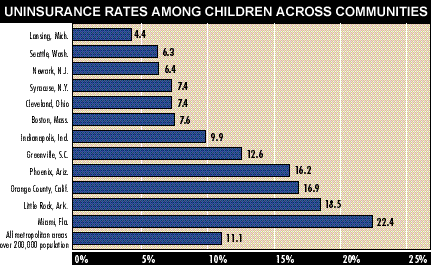
The four factors that consistently explain the greatest variation across the 12 communities, in descending levels of importance, are:
- the percentage of parents with an offer of insurance from their employer;
- the percentage of children from Spanish-speaking families;
- the percentage of Medicaid-eligible children; and
- the distribution of income among families with children.
These four factors clearly are related to the four reasons children go without health insurance. Offer rates by employers are closely tied to whether parents lack access to employer-sponsored insurance. For example, only 54 percent of children in Miami have a parent who is offered health insurance through an employer. This compares with 73 percent among children nationally. If offer rates in Miami increased to equal the national average, children’s uninsurance rate would decline by four percentage points.
Even after accounting for different income levels, insurance offer rates and other factors, Hispanic children are the group most likely to be uninsured. More than one in four lack health insurance. However, it is the language barrier, rather than being of Hispanic ethnicity, that predominantly affects uninsurance rates among these children. Higher than average percentages of Spanish-speaking families contribute to the high uninsurance rates among children in Miami and Orange County.
Within federal guidelines, states have considerable discretion in setting Medicaid eligibility levels. Prior to the enactment of CHIP, variations in state Medicaid eligibility rules for children accounted for as much as a two percentage point variation in the overall uninsurance rate among children in the 12 sites.
Income distribution among lower-income families living in cities, particularly the percentage living in poverty, explains a significant portion of the variation in local uninsurance rates among children. Concentrations of poor children in Little Rock and Miami account for some of the relatively high rates of uninsurance among children there. Because HSC’s estimates control for local variations in Medicaid eligibility and employer offer rates, one explanation of why there are more uninsured children in these sites is that lower-income persons are less likely to enroll in private insurance even when it is available.
Policy Responses
![]() HIP has the potential to significantly reduce the number of uninsured children in the United States. To achieve CHIP’s full potential, however, states must be creative and aggressive in their efforts to identify and recruit eligible children.
HIP has the potential to significantly reduce the number of uninsured children in the United States. To achieve CHIP’s full potential, however, states must be creative and aggressive in their efforts to identify and recruit eligible children.
There are several ways in which states can design their health insurance program to reach children who are without insurance due to their parents experiencing a gap in coverage, because of a job transition or some other reason. States can:
- direct outreach activities to unemployment offices;
- refrain from imposing waiting periods for CHIP coverage for children who become uninsured because their parents lose or change jobs;
- cover children for 12 months, even if the children no longer meet eligibility criteria due to changes in family income and other factors;
- consider insurance market reforms that limit or eliminate waiting periods for new employees and limit the ability of firms to deny coverage to part-time workers and those with preexisting conditions; and
- develop policies, such as portability provisions, that ensure continuity of coverage.
Under Medicaid, states are able to pay the premiums, deductibles and copayments of Medicaid beneficiaries with private insurance coverage when it is cost-effective to do so. Few states have taken advantage of this option because of administrative issues, such as identifying beneficiaries with private coverage options. Eligibility under CHIP is extended to higher-income children whose parents are more likely to have offers from their employers, so more states might be willing to look into this approach.
Many states have enacted or are considering enacting measures to reduce the stigma associated with receiving public health insurance by making Medicaid and CHIP look as much like private insurance as possible. Many are also attempting to streamline eligibility determinations.
Apart from these overall efforts, states recognize that they will need to seek out families with eligible children. The following are two specific targets for outreach efforts.
Hispanic Families
Forty percent of uninsured Medicaid-eligible children are Hispanic, and children potentially eligible for CHIP are twice as likely to be Hispanic as the general population of children. This suggests that outreach efforts should be directed toward neighborhoods with large Hispanic populations and Hispanic social, religious and cultural institutions.
Sensitivity to language barriers is quite important. Hispanic Medicaid-eligible children of persons not fluent in English are far more likely than those with parents fluent in English to be uninsured. This suggests that language is a major barrier to enrollment and may be related to both knowledge and acceptance of public insurance. It may also indicate the family’s immigration status, a potential legal barrier to gaining coverage.
Health Care Settings
Only one uninsured child in five does not have a usual source of care. Although it is reasonable to assume that emergency rooms, hospital outpatient clinics and public clinics regularly inform uninsured patients of their public insurance options, it is not clear that physicians in private practice actively do so. About a third of uninsured children who are Medicaid-eligible use a doctor’s office as their usual source of care. Among children potentially eligible for CHIP, the proportion grows to 41 percent. This suggests that states might encourage physicians to participate in outreach efforts.
Only one uninsured child in five does not have a usual source of care. Although it is reasonable to assume that emergency rooms, hospital outpatient clinics and public clinics regularly inform uninsured patients of their public insurance options, it is not clear that physicians in private practice actively do so. About a third of uninsured children who are Medicaid-eligible use a doctor’s office as their usual source of care. Among children potentially eligible for CHIP, the proportion grows to 41 percent. This suggests that states might encourage physicians to participate in outreach efforts.
Note 1
![]() he target population for CHIP includes children under age 19 in families with incomes less than 200 percent of the federal poverty level or 50 percentage points above the state’s income eligibility levels as of August 22, 1997. Some states have expanded eligibility beyond these income levels.
he target population for CHIP includes children under age 19 in families with incomes less than 200 percent of the federal poverty level or 50 percentage points above the state’s income eligibility levels as of August 22, 1997. Some states have expanded eligibility beyond these income levels.
Survey Methodology
![]() ata for this Issue Brief are from the 60-site Household Survey, conducted as a part of HSC’s Community Tracking Study to monitor changes in the health care system over time and to gain a better understanding of how health system changes affect both consumers and providers. Surveys of physicians, employers and health plans, and site visits to 12 of the communities are also being conducted as part of the study. Surveys and site visits will mostly be conducted in two-year cycles.
ata for this Issue Brief are from the 60-site Household Survey, conducted as a part of HSC’s Community Tracking Study to monitor changes in the health care system over time and to gain a better understanding of how health system changes affect both consumers and providers. Surveys of physicians, employers and health plans, and site visits to 12 of the communities are also being conducted as part of the study. Surveys and site visits will mostly be conducted in two-year cycles.
The Household Survey was conducted by telephone interviews and in-person interviews of families in households without a telephone between July 1996 and July 1997. The file used for this analysis contains observations on over 60,000 individuals and nearly 33,000 families. About 11,600 of these families have children. Questions were asked about insurance coverage, health status, access to and utilization of health care, satisfaction with the health care system and demo-graphic characteristics. The data are weighted to be representative of the U.S. population.
More on CHIP
![]() he first issue of HSC’s Research Report features the complete text of "CHIPing Away at the Problem of Uninsured Children: Why Children Lack Health Insurance and Implications for the New State Children’s Health Insurance Programs," from which this Issue Brief is adapted. This new series begins publication in September.
he first issue of HSC’s Research Report features the complete text of "CHIPing Away at the Problem of Uninsured Children: Why Children Lack Health Insurance and Implications for the New State Children’s Health Insurance Programs," from which this Issue Brief is adapted. This new series begins publication in September.