
Local Innovations Provide Managed Care for the Uninsured
Issue Brief No. 25
January 2000
Laurie E. Felland, Cara S. Lesser
![]() number of communities in the United States are
adopting a managed care approach to caring for low-income
uninsured individuals. This Issue Brief focuses on such
programs in five of the 12 communities that the Center for
Studying Health System Change (HSC) is tracking intensively.
It describes the local market factors that motivated the
creation and varying design of these initiatives, all of
which seek to increase access to primary and preventive care
while managing the use of more costly inpatient and emergency
care. The Issue Brief also discusses the long-term viability
of these programs as they attempt to simultaneously expand
access to services and contain costs for this growing
population.
number of communities in the United States are
adopting a managed care approach to caring for low-income
uninsured individuals. This Issue Brief focuses on such
programs in five of the 12 communities that the Center for
Studying Health System Change (HSC) is tracking intensively.
It describes the local market factors that motivated the
creation and varying design of these initiatives, all of
which seek to increase access to primary and preventive care
while managing the use of more costly inpatient and emergency
care. The Issue Brief also discusses the long-term viability
of these programs as they attempt to simultaneously expand
access to services and contain costs for this growing
population.
Providing Managed Care for the Uninsured
![]() ecent
changes in the American health care system have exacerbated
the challenge of caring for the uninsured. Of the
approximately 44 million uninsured, roughly half are
considered low-income, with annual earnings of less than 200
percent of the federal poverty level. These individuals
generally lack access to preventive and primary care and rely
instead on episodic medical treatment that is supported
through a patchwork of government programs and
cross-subsidies from the insured. Market changes-and the
growth of managed care in particular-have increased pressure
on these resources, yet also have inspired new ideas for
meeting the health needs of the uninsured.
ecent
changes in the American health care system have exacerbated
the challenge of caring for the uninsured. Of the
approximately 44 million uninsured, roughly half are
considered low-income, with annual earnings of less than 200
percent of the federal poverty level. These individuals
generally lack access to preventive and primary care and rely
instead on episodic medical treatment that is supported
through a patchwork of government programs and
cross-subsidies from the insured. Market changes-and the
growth of managed care in particular-have increased pressure
on these resources, yet also have inspired new ideas for
meeting the health needs of the uninsured.
Managed care programs for the uninsured are being established in communities across the country as an innovative way to improve health status and control costs. They provide more preventive and primary services while managing the use of more expensive inpatient and emergency care. In general, the programs use existing charity care funding to provide health care to low-income uninsured individuals who are not eligible for public insurance programs. The initiatives often resemble Medicaid expansions, but because they are not entitlements and rely on limited local funding, they do not provide the same guaranteed benefits as insurance.
Five of the 12 communities that HSC studies have some form of managed care program for the uninsured. Boston, Indianapolis and Lansing have had such programs for at least one year, and Orange County, Calif., and Northern New Jersey are exploring pilot projects (see box below).
Market Changes Spur New Programs
A variety of local market changes have motivated the development of managed care programs for the uninsured across the HSC study sites. The five markets have diverse characteristics that historically have affected how they provide care for low-income uninsured individuals (see Figure 1). Despite these differences, providers and policy makers in each community now have adopted a managed care approach. While the general strain on resources is a motivating factor, specific changes have acted as catalysts for these programs, including the introduction of Medicaid managed care, hospital mergers and deregulation of hospital rates.
Medicaid Managed Care. Managed care programs for the uninsured were developed in some communities in response to the rapid growth of Medicaid managed care (see Figure 2). There was concern that the transition to managed care would strain safety net providers’ financial resources available to care for the uninsured. In addition, because many low-income individuals cycle in and out of Medicaid due to changes in their eligibility status, providers and policy makers have turned to a managed care model for the uninsured in an effort to foster continuity.
In 1995, Massachusetts authorized Boston’s largest safety net providers, Boston Medical Center and Cambridge Health Alliance, to use charity care funds to create managed care programs for the uninsured who were expected to become eligible for Medicaid through planned expansions. Ultimately, eligibility was not expanded as much as projected, but the safety net hospitals maintained the Boston HealthNet and Network Health programs for the uninsured and created separate Medicaid programs with similar names.
Similarly, in Michigan, concerns about Medicaid managed care’s potential strain on the safety net motivated the local health department to develop a plan to enroll all residents in an organized system of health care by 2005. This goal, along with funding assistance from the state, inspired the Ingham County Health Department in Lansing to create the Ingham Health Plan for the county’s low-income uninsured residents in 1998.
In 1995, Orange County moved to Medicaid managed care under the direction of a local agency, CalOPTIMA. It was expected that CalOPTIMA would integrate the county’s Medical Services for the Indigent (MSI) program once Medicaid beneficiaries were enrolled. However, CalOPTIMA has been concerned that funding is insufficient to provide the MSI eligibles with the same comprehensive benefits that the Medicaid enrollees receive. As an interim step, the agency has proposed integrating a limited number of chronically ill MSI beneficiaries to learn more about the health care needs and utilization patterns of a population that program administrators expect to be the most challenging to incorporate into a managed care model.
Hospital Mergers. Although expansion of Medicaid managed care also played a role in Indianapolis, the merger of two major hospitals into Clarian Health was one of the key forces motivating the development of the Wishard Advantage Program. Wishard Hospital, Indianapolis’s public hospital, was not involved in the merger and was worried that its capacity to care for the uninsured would be challenged as Clarian used its leverage to compete for Medicaid beneficiaries and integrated physicians who traditionally served the uninsured.
Deregulation. State deregulation of hospital rates and the associated change in traditional models of charity care funding contributed to the development of managed care programs for the uninsured in Boston and New Jersey. Safety net providers became uneasy that private hospitals would underbid them for health plan business and leave them with reduced revenue to subsidize charity care.
In response to these concerns, the New Jersey state legislature attempted to redesign charity care into a hospital-based managed care system. In effect, this would require hospitals statewide to cover comprehensive primary and preventive services through a coordinated provider network. Some hospitals lobbied against this plan because it required them to allocate a portion of their already strained disproportionate share hospital (DSH) revenues to unaffiliated outpatient providers. The proposal was subsequently scaled back to the Managed Charity Care Demonstration, a pilot project that allows voluntary hospital participation. This revised model is under review by the Health Care Financing Administration because it still involves redirecting DSH funds to cover services provided outside the hospital setting.
Figure 1
Market Characteristics of Five Sites with Managed Care for the Uninsured
| Boston | Indianapolis | Lansing | Northern New Jersey | Orange County | Average for Metropolitan Areas with over 200,000 population | |
| HMO Pene- tration1 |
49% | 23% | 41% | 24% | 46% | 34% |
| Persons Living in Poverty2 | 10 | 10 | 11 | 10 | 15 | 15 |
| Persons with No Health
Insur- ance2 |
9.1 | 11 | 8.3 | 9.8 | 16 | 14 |
| Percent Uninsured Reporting Difficulty in Getting Health Care2 | 33 | 35 | 41 | 25 | 19 | 30 |
Sources:
1. InterStudy Competitive Edge 8.2, 1998
2. HSC Community Tracking Study Household Survey, 1996-1997
Figure 2
|
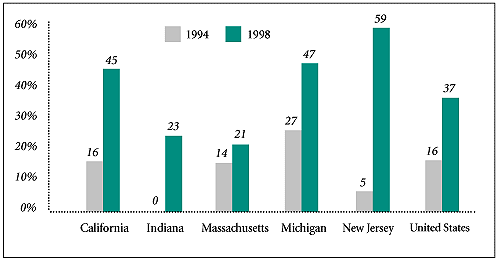 |
Source: Medicaid Managed Care: A Guide for States, 2nd and 4th Editions, National Academy of State Health Policy, 1994 and 1998
Diverse Program Structure
![]() he
five programs share a number of managed care features,
including the use of primary care physicians to coordinate
utilization of services within an established provider
network and mechanisms to control costs. However, they vary
in the scope of services offered, populations targeted,
funding sources and approaches to provider reimbursement.
he
five programs share a number of managed care features,
including the use of primary care physicians to coordinate
utilization of services within an established provider
network and mechanisms to control costs. However, they vary
in the scope of services offered, populations targeted,
funding sources and approaches to provider reimbursement.
Provider Networks. Most of the programs have developed around local safety net hospitals, relying on their ambulatory facilities to provide preventive and primary care. Many have also affiliated with local community health centers and other providers to expand capacity. For example, Ingham Health Plan in Lansing plans to contract with private practitioners as the community health centers reach capacity. Others have been reluctant to collaborate with community-based providers. Some New Jersey hospitals, for example, have raised concerns that these partnerships would dilute their already limited resources to care for the uninsured.
Scope of Services. HSC found that the scope of services provided by the managed care programs varied widely. At one end of the spectrum are Boston’s programs, which provide comprehensive inpatient and outpatient coverage. At the other end is Ingham Health Plan, which covers only outpatient services. The programs strive to provide needed health services without offering benefits more attractive than those of public insurance programs, and proactively transfer enrollees to Medicaid or the federal Children’s Health Insurance Program if they become eligible.
The initiatives seek to modify enrollees’ care-seeking patterns and encourage their use of preventive and primary care. Expanded clinic hours and 24-hour medical help lines are established to facilitate outpatient care in lieu of emergency care when possible. Additional program features include social services to improve access, such as language interpreters and reduced-cost transportation to health care facilities.
However, the extent to which the programs aggressively manage care varies. In Lansing, Ingham Health Plan enrollees must get referrals for specialty care. In contrast, the Boston initiatives do not restrict access or utilization, although they do attempt to reroute patients to outpatient settings for nonurgent care. Wishard Advantage Program in Indianapolis initially implemented a pre-authorization process, but abandoned it due to insufficient infrastructure and the fact that enrollees did not tend to self-refer for specialty or ancillary services. Nevertheless, both Wishard and New Jersey’s proposed program maintain some degree of provider utilization management.
Population Enrolled. The managed care initiatives are generally intended for low-income, uninsured individuals who are ineligible for public insurance. The lowest-income enrollees-ranging from below 100 percent of the federal poverty level in Lansing to below 200 percent in Boston, Orange County and New Jersey-do not face cost-sharing requirements for services, while individuals above those ranges pay on a sliding scale in some sites. Some of the programs provide partial benefits to those with limited insurance coverage. Health status is generally not a factor for eligibility, although both the New Jersey and Orange County pilots plan to target individuals with certain diagnoses.
The programs range in size from 1,000 enrollees for the pilot program in Orange County to an estimated 73,000 enrollees for the two Boston programs combined. In general, enrollees are single adults, and many are reportedly employed. In fact, the Ingham County Health Department is now considering plans to target this population explicitly by marketing the Ingham plan to small employers.
Attempts to reach the target population vary considerably by program. In some sites, individuals learn about the program only when they go to a clinic or hospital for medical care. Other programs automatically enroll individuals from an existing indigent program and actively seek out potential enrollees in the community. In the programs that have been implemented, enrollees receive a membership card resembling a standard insurance card to facilitate access to services.
Funding. Funding for the managed care programs identified in HSC’s sites comes from existing indigent funds from federal, state and local sources. Most participating hospitals dedicate a portion of their federal DSH funds to the programs. Indianapolis and Lansing also use county tax revenues, and Boston relies on a portion of funds from the state uncompensated care pool, a fund generated by hospitals and health plans to reimburse charity care providers.
Provider Reimbursement. Most of the programs use risk-based payment mechanisms to help control expenditures. For example, outpatient providers of the Wishard Advantage Program receive a capitated payment of $15 per member per month, while Wishard Hospital bears the risk for ancillary and inpatient services. The Ingham Health Plan also provides capitated payments to participating providers. In contrast, providers in the Boston programs are paid on a fee-for-service basis. However, state policy makers and program administrators are considering implementing partial risk-bearing arrangements to reduce strain on the uncompensated care pool.
Program administrators are faced with the challenge of offering competitive provider reimbursement while also controlling expenditures. Overall, they report that payments are generally comparable to, if not better than, those of Medicaid and other managed care payers. As a result, the established programs have little if any difficulty in recruiting and retaining providers. In addition, because the programs rely heavily on hospital-based DSH funds, providers not affiliated with local hospitals may be eager to participate to capture new revenues.
At a Glance: Programs for the Uninsured in Three Communities
| Boston HealthNet and Network Health Programs, Boston, Mass. | Wishard Advantage Program, Indianapolis, Ind. | Ingham Health Plan, Lansing, Mich. | ||
| Implementation: 1995 | Implementation: 1997 | Implementation: 1998 | ||
| Services: Outpatient primary and specialty, inpatient, emergency, ancillary, limited dental, vision, pharmacy and mental health | Services: Outpatient primary and specialty, inpatient, emergency, ancillary, pharmacy, limited mental health | Services: Outpatient primary and specialty, ancillary, pharmacy | ||
| Eligibility: Less than 200 percent of federal poverty level receive free care | Eligibility: Less than 150 percent of federal poverty level receive free care; less than 200 percent of federal poverty level have cost-sharing requirements | Eligibility: Less than 100 percent of federal poverty level receive free care; less than 250 percent of federal poverty level have cost-sharing requirements | ||
| Enrollment: Boston HealthNet 62,000; Network Health 11,000 | Enrollment: 20,000 | Enrollment: 8,500 | ||
| Funding: Drawn from state uncompensated care pool and DSH; amount varies according to demand for services | Funding: $56 million annually from city and county property tax revenues | Funding: $3.5 million annually from DSH, Medicaid, county tax revenues | ||
| Provider Reimbursement: Fee-for-service | Provider Reimbursement: Capitated payment of $15 per member per month for primary care; varied arrangements for specialty and inpatient services | Provider Reimbursement: Global capitated payment of $24 per member per month | ||
| Note: Programs in two other HSC study sites-Orange County, Calif., and Northern New Jersey-are in development and have not yet been implemented. | ||||
Looking Ahead
![]() ecause the
managed care programs in the HSC sites are relatively new, it
is difficult to draw conclusions about their ability to
improve health care outcomes for the uninsured. However, some
of the programs have already shown progress toward their
goals. For example, the Wishard Advantage Program has cut
annual inpatient days in half and reduced emergency room use
by 30 percent among its enrollees, and Boston Medical Center
has decreased emergency room use for its uninsured population
enrolled in the Boston HealthNet program.
ecause the
managed care programs in the HSC sites are relatively new, it
is difficult to draw conclusions about their ability to
improve health care outcomes for the uninsured. However, some
of the programs have already shown progress toward their
goals. For example, the Wishard Advantage Program has cut
annual inpatient days in half and reduced emergency room use
by 30 percent among its enrollees, and Boston Medical Center
has decreased emergency room use for its uninsured population
enrolled in the Boston HealthNet program.
However, the intent to both expand access to care and control costs raises some concerns. Many policy makers and safety net providers are hesitant to assume that the increased demand for outpatient services will be offset by a decrease in costs from reduced emergency and inpatient care utilization, and they fear that expenditures may actually rise as additional services are offered to more people. In fact, some program directors do not believe that the programs will save money because they must compensate for the previous dearth of specialty and tertiary medical services-as well as primary care-for this population.
In programs that incorporate explicit assumptions of cost reductions, the parties at risk for the anticipated savings are often apprehensive. For example, New Jersey hospitals and CalOPTIMA in Orange County are concerned that they will be responsible for offering comprehensive services with insufficient reimbursement. Without knowing more about the health care needs of the uninsured populations in their community, providers are uncertain that increased preventive services will ultimately generate savings and are reluctant to bear the related financial risk, especially if they are required to surrender funds to other providers in the process.
All of the programs have expressed concern about the adequacy of funding. If funds are depleted, participating providers could be left with the responsibility of providing needed medical services and absorbing the additional costs. In this respect, the programs ultimately function more like uncompensated care pools than public insurance programs because they include no legal commitment to reimburse providers for a contracted set of benefits. This is especially troubling to providers that face deteriorating margins and worry about their ability to support the cost of this care through traditional cross-subsidies.
From the enrollees’ perspective, this lack of guarantee to cover a broad spectrum of services also distinguishes the programs from insurance. If the programs deplete their funds, individuals could be disenrolled or have their benefits reduced. This could push them back into the traditional, fragmented charity care system. To avoid such an outcome and to ensure long-term sustainability, advocates for the managed care initiatives contend that additional funding is needed. Program directors acknowledge the inherent fragility of their programs by helping enrollees to obtain more stable public or private insurance when possible.
Regardless of these limitations, these programs have many potential benefits. They may help provide a usual source of care for the uninsured and improve local knowledge of the health care needs of this population. In addition, the programs may channel individuals toward more cost-effective care settings by encouraging and increasing access to preventive and primary care services. This could reduce the risk and cost of serving this population, and thereby expand access to insurance coverage.
Ultimately, the extent to which managed care programs result in such outcomes remains to be seen. Nevertheless, the successes and limitations of these programs will provide important insights for policy makers as they grapple with the challenge of caring for the growing uninsured population in a changing health care environment.
HSC’s Sites
![]() he Community
Tracking Study, the major effort of HSC, tracks changes in
the health system in 60 sites that are representative of the
nation. Every two years, HSC conducts surveys in all 60
communities and site visits in the following 12 communities:
Boston, Mass.; Cleveland, Ohio; Greenville, S.C.;
Indianapolis, Ind.; Lansing, Mich.; Little Rock, Ark.; Miami,
Fla.; Northern New Jersey; Orange County, Calif.; Phoenix,
Ariz.; Seattle, Wash.; and Syracuse, N.Y.
he Community
Tracking Study, the major effort of HSC, tracks changes in
the health system in 60 sites that are representative of the
nation. Every two years, HSC conducts surveys in all 60
communities and site visits in the following 12 communities:
Boston, Mass.; Cleveland, Ohio; Greenville, S.C.;
Indianapolis, Ind.; Lansing, Mich.; Little Rock, Ark.; Miami,
Fla.; Northern New Jersey; Orange County, Calif.; Phoenix,
Ariz.; Seattle, Wash.; and Syracuse, N.Y.
The first round of site visits took place in 1996 and 1997, the second round in 1998 and 1999. The findings reported in this Issue Brief are based on the second round of site visits, which are available at www.hschange.com.
ISSUE BRIEFS are published by Health System Change.
President: Paul B. Ginsburg
Director of Public Affairs: Ann C. Greiner
Editor: The Stein Group