Do HMOs Make a Difference?
Comparing Access, Service Use and Satisfaction Between Consumers in HMOs and Non-HMOs
Issue Brief No. 28
March 2000
James D. Reschovsky, Peter Kemper, Ha T. Tu, Timothy K. Lake, Holly L. Wong
![]() he growth of managed care has prompted questions about the effects of health
maintenance organizations (HMOs) on consumers. This Issue Brief reports the results from a
large national study of the privately insured population. No detectable difference was
found between HMOs and other types of insurance in the use of three costly
services-inpatient care, emergency room use and surgeries-and differences in reports of
unmet need or delayed care are negligible. Differences for other measures pose a trade-off
for consumers: HMOs provide more primary and preventive services and lower financial
barriers to care, but they provide less specialist care and raise administrative barriers
to care. In addition, patients in HMOs report less satisfaction, less trust in physicians
and lower ratings of physician visits. These findings have implications for the current
policy debate about managed care.
he growth of managed care has prompted questions about the effects of health
maintenance organizations (HMOs) on consumers. This Issue Brief reports the results from a
large national study of the privately insured population. No detectable difference was
found between HMOs and other types of insurance in the use of three costly
services-inpatient care, emergency room use and surgeries-and differences in reports of
unmet need or delayed care are negligible. Differences for other measures pose a trade-off
for consumers: HMOs provide more primary and preventive services and lower financial
barriers to care, but they provide less specialist care and raise administrative barriers
to care. In addition, patients in HMOs report less satisfaction, less trust in physicians
and lower ratings of physician visits. These findings have implications for the current
policy debate about managed care.
Debate about HMOs
![]() nrollment in HMOs has grown tremendously
over the past decade, now accounting for more than half of all privately insured persons.
Although HMOs and other managed care plans have been credited with controlling costs, both
consumers and providers are questioning whether, as a result, care is being compromised.
Consumer concerns about restrictions on the choice of providers, limits on the
availability of services and the quality of health care have sparked a managed care
backlash and generated support for government regulation of managed care in general and
HMOs in particular.
nrollment in HMOs has grown tremendously
over the past decade, now accounting for more than half of all privately insured persons.
Although HMOs and other managed care plans have been credited with controlling costs, both
consumers and providers are questioning whether, as a result, care is being compromised.
Consumer concerns about restrictions on the choice of providers, limits on the
availability of services and the quality of health care have sparked a managed care
backlash and generated support for government regulation of managed care in general and
HMOs in particular.
Industry defenders argue that unfavorable press reports about substandard care in HMOs often are based on unrepresentative cases, while the typical experience goes unreported. They assert that HMOs’ greater emphasis on prevention and care management results in better, more cost-effective care than less managed types of insurance can offer.
Much of the debate, however, has been hampered by a lack of current empirical evidence concerning health care under HMOs. This study attempts to narrow this information gap by systematically comparing how HMOs affect their enrollees’ access to care, use of health care services and satisfaction with care with those not enrolled in HMOs.
Analysis of HMOs’ Effects
![]() hile much has been published
comparing aspects of care provided to patients in HMO and other, non-HMO insurance, such
as preferred provider organizations (PPOs) and traditional fee-for-service insurance, it
remains difficult to draw general conclusions from this body of research. Results from
different studies frequently provide inconsistent or inconclusive results because of
differences in the data and methodology used. Data are often out-of-date, and samples
frequently represent narrow populations, such as members of a small number of health plans
or residents of a single city. Studies vary in their methodology, particularly their
ability to control for differences in people enrolled in HMOs and other types of
insurance. Finally, most studies examine only a narrow set of measures of HMOs’ effects.
hile much has been published
comparing aspects of care provided to patients in HMO and other, non-HMO insurance, such
as preferred provider organizations (PPOs) and traditional fee-for-service insurance, it
remains difficult to draw general conclusions from this body of research. Results from
different studies frequently provide inconsistent or inconclusive results because of
differences in the data and methodology used. Data are often out-of-date, and samples
frequently represent narrow populations, such as members of a small number of health plans
or residents of a single city. Studies vary in their methodology, particularly their
ability to control for differences in people enrolled in HMOs and other types of
insurance. Finally, most studies examine only a narrow set of measures of HMOs’ effects.
This study addresses these earlier shortcomings. It uses data from a large, nationally representative sample of privately insured persons under age 65. The data, which were collected in 1996 and 1997, are among the most recent available. In addition, the study’s scope is broad, encompassing numerous measures of access, service use and consumer assessments of care. By employing a consistent data source and methodology, we are able to draw conclusions about HMO effects across three areas of inquiry:
- Access to care includes measures of unmet need for care and financial and administrative barriers to care.
- Service use includes ambulatory visits of various types (physicians, nonphysician practitioners and emergency rooms), whether the last visit was to a specialist, hospital use, surgeries and preventive services such as mammograms.
- Consumers’ assessments of care include satisfaction with overall health care and choice of physicians, ratings of patients’ last doctor visit and patients’ trust in their physicians.
The range of measures allows us to provide a comprehensive picture of HMO performance across multiple dimensions and identify trade-offs among HMOs’ effects. However, it is not sufficient simply to compare performance measures between persons in the two types of insurance, because the population in HMOs might differ from the population not in HMOs. To avoid bias, we controlled for a wide range of enrollee characteristics, such as health status and income, that might otherwise bias the comparisons (see Data Sources and Methodology).
Little Difference Found on Some Important Dimensions
![]() he study did not find evidence of
differences between HMOs and other types of insurance in hospital use, emergency room
visits or surgeries. In addition, reports of unmet need or delayed care, important
indicators of access to care, differ little between HMO enrollees and people with other
types of insurance.
he study did not find evidence of
differences between HMOs and other types of insurance in hospital use, emergency room
visits or surgeries. In addition, reports of unmet need or delayed care, important
indicators of access to care, differ little between HMO enrollees and people with other
types of insurance.
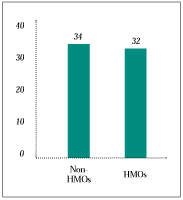
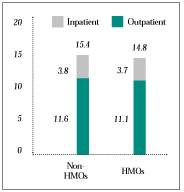
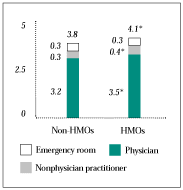
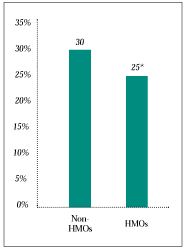
Hospital, Surgery and Emergency Room Use. Comparing use of costly services in HMOs with that in other forms of insurance is important because of the interest in controlling health care costs and concern about access to these services. The study did not find evidence of reduced use of three important services under HMOs. The difference between HMO enrollees’ hospital use and that of people with other types of insurance is small and not statistically significant (see Figure 1). Overall use of surgery does not differ significantly, nor is there evidence of greater reliance on outpatient over inpatient surgery in HMOs (see Figure 2). We also found no evidence that HMO enrollees use emergency rooms less frequently. Among the costly services examined in this study, only specialty services are delivered to HMO enrollees less frequently than to others.
Findings regarding hospital, emergency room and surgery use are important, not only because these services are costly, but also because these findings are contrary to conventional wisdom about where HMOs have cut costs. This can be explained in two ways.
First, the estimates reported here reflect HMO effects at the individual level. They do not include any systemwide effects of HMOs on care delivery. If the increase in HMO market share over time has affected how providers treat all patients, not just those in HMOs, then these spillover effects may have diminished HMO/non-HMO differences at the individual level.
Second, driven by competitive market pressures, HMOs and other products have become more similar over time. Traditional fee-for-service and PPO products have adopted some managed care tools originally developed by HMOs, such as preadmission authorization for nonemergency hospital care. At the same time, HMOs have responded to competitive pressure by offering products with broader networks and out-of-network coverage. As traditional fee-for-service insurance has lost market share and the HMO/non-HMO product differences have diminished, individual-level HMO effects may well have decreased correspondingly.
Although the results of this study should be encouraging for those concerned that HMOs may stint on costly but necessary care, they may not be so encouraging for those who see HMOs as the way to control health care costs by reducing inappropriate care or shifting care to appropriate but less costly settings. HMOs have been credited with bringing health care cost increases under control, and they have done so at least in part by negotiating discounted rates for providers. In the long run, however, control of costs-without reducing benefits-will depend on care management tools and more efficient use of services. Yet, implementation of the more sophisticated of these tools-and the information systems needed to support them-has been slow.
It is important to point out that the nature and efficacy of the care received by individuals in the survey is not known. The content of a visit, the surgical procedure used or the quality of care provided could be affected for better or worse without changing the number of patient days, surgeries or emergency room visits. In addition, the study did not include measures of other costly services, such as tests and nonsurgical procedures.
Unmet Needs or Delayed Care. Public opinion polls suggest that many consumers are concerned about whether HMOs will provide the care they need when they become sick. Access to care matters because care management tools and financial incentives to providers designed to constrain use of unnecessary services also may constrain access to needed care. At the same time, other attributes associated with HMOs may promote care seeking on the part of patients. These include low cost sharing, 24-hour outpatient clinics and reminder systems for preventive care services.
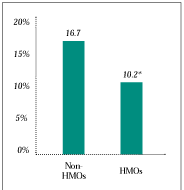
The study found that HMO enrollees are only slightly more likely than enrollees in other plans to report that they did not get care they thought they needed, and the study found no evidence of differences in reports of delayed care needs (see Figure 3). Among other indicators of access-how long it takes to get an appointment, travel time to get care and waiting time in the office-there was no evidence of differences between types of insurance.
Figure 1
|
Figure 2
|
Consumers Face Trade-Offs on Other Dimensions
![]() he study did find differences between
HMOs and other types of insurance that pose important trade-offs for consumers. HMOs lower
financial barriers to care, but raise administrative ones. HMOs also increase ambulatory
and preventive care, but reduce specialist care. HMO enrollees’ overall assessments of
care are lower than those of people with other types of insurance.
he study did find differences between
HMOs and other types of insurance that pose important trade-offs for consumers. HMOs lower
financial barriers to care, but raise administrative ones. HMOs also increase ambulatory
and preventive care, but reduce specialist care. HMO enrollees’ overall assessments of
care are lower than those of people with other types of insurance.
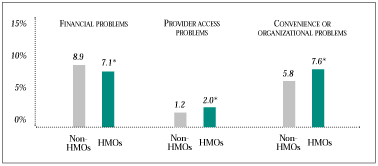
Barriers to Care. Out-of-pocket costs for health care are lower for HMO enrollees (see Figure 4). As a consequence, HMO enrollees are less likely to report unmet or delayed care needs because of financial concerns. On the other hand, HMO enrollees are more likely to report unmet or delayed care needs related to administrative problems (see Figure 5). These include provider access problems (e.g., difficulty obtaining a referral or attempting to receive care from a provider not included in their health plan’s network) and convenience or organizational problems (e.g., difficulties getting an appointment soon enough).
These differences follow directly from the different approaches HMOs and other types of insurance use to limit the amount of health care their enrollees use. Lower out-of-pocket costs and fewer financial barriers to care are consistent with HMOs’ reliance on modest copayments rather than the more costly coinsurance and deductibles common among traditional fee-for-service insurance and PPOs. Instead of relying on these consumer financial incentives to influence care decisions, HMOs rely on provider-focused tools, such as use of narrower networks, restrictions on out-of-network coverage, providers’ financial incentives and utilization management-including gatekeeping- to manage care.
Ambulatory Care. The study found that, as expected, HMOs increase ambulatory and preventive care but reduce specialist care. Compared with people with other types of insurance, HMO enrollees:
make more visits to physician and nonphysician practitioners; however, no difference was found in emergency room visits (see Figure 6);
are more likely to have a regular place where they receive health care;
are more likely to obtain preventive care, as indicated by receipt of flu shots and, for women over 40, mammograms; however, no difference was found in receipt of advice from physicians to quit smoking (see Figure 7).; and
make fewer visits to specialists (see Figure 8).
These differences also flow from design differences between HMOs and other types of insurance. Greater use of primary care physicians and greater likelihood of having a usual source of care, for example, are consistent with HMOs’ orientation toward care management and emphasis on primary care. HMO enrollees are more likely to have a primary care physician who coordinates care and serves as a gatekeeper, making decisions about when specialist care is required. The greater number of total ambulatory care visits found in HMOs may reflect lower cost sharing among HMO enrollees, provision of more primary care or the need to visit a gatekeeper to obtain access to specialist care.
Finally, because specialist care is more expensive than primary care, the use of less specialty care in HMOs provides an important avenue through which HMOs may achieve cost savings. Not only are specialist visits more costly than primary care physician visits, but specialists often are more likely to use costly tests and procedures.
Consumer Assessments. Although individuals’ assessments of health care along the three dimensions examined are generally quite high regardless of their insurance coverage, HMO enrollees’ assessments of care, with one exception, are lower than those among people who are not in HMOs (see Figure 9).
- HMOs receive lower patient ratings with respect to doctors’ listening, explanation and thoroughness on their last visit.
- HMO enrollees are less likely to trust that their doctor will put medical needs first and that he or she will refer them to a specialist when needed. However, HMO enrollees express the same level of concern about their doctor performing unnecessary tests or procedures.
- Satisfaction with choice of primary care physicians and specialists and overall satisfaction with health care are all lower among HMO enrollees.
There are several possible explanations for these findings. Some dissatisfaction may be due to the intrusion of care management tools such as obtaining permission for tests and procedures. Required referrals and the absence of out-of-network coverage, for example, are all apparent to consumers and may create real or perceived barriers to obtaining care-regardless of their effect on the care itself.
Perceived or actual restrictions on the use of specialist care may be of particular concern for patients. Indeed, satisfaction with choice of specialists and trust in physicians’ willingness to refer to specialists are the two assessments on which HMOs fared worst. Not having control over being able to see specialists may be one of the most visible and difficult adjustments for those accustomed to PPO or traditional fee-for-service insurance.
Consumer dissatisfaction also may be derived in part from physicians’ discontent with managed care, which may stem from the imposition of the tools used by managed care, managed care’s effect on physicians’ compensation or its effects on care delivery and quality. Some physicians undoubtedly share their concerns with their patients.
Other researchers have offered another potential explanation. Although the overwhelming majority of people in HMOs are very satisfied with their care, public opinion polls indicate that a majority of the general public feels that HMOs would not provide all the care needed in the event of a serious illness. These attitudes-and the resulting effect they may have on assessments of care-may be driven by anecdotes heard from a friend or read in the press, rather than by personal experience. Thus, a few visible cases where patients do not receive needed care can lead to widespread unfavorable assessments, even if the vast majority of HMO enrollees’ own experiences are positive. In fact, since only one half of one percent of HMO enrollees report not being able to see a specialist as a reason for not receiving or having to delay needed care, the public appears to view the risk of being denied access to a specialist for needed care as being greater in an HMO than is likely the case.
Finally, some of the consumer dissatisfaction with managed care could be transitional. To the extent that dissatisfaction is due to inexperience obtaining care in a managed care system, dissatisfaction might diminish over time as patients learn how such a system works.
In interpreting these findings, it is important to underscore that consumer assessments are not measures of clinical quality. Information about the content of a visit, the course of treatment, type of surgery, clinical aspects of care and other details cannot be obtained from telephone surveys. It is common for patients to assume that more care is equivalent to better quality care, but that is not always true. For example, it is unclear how the substitution of primary for specialist care affects clinical quality. Consumers may perceive less access to specialists as lower quality. Yet, if too much specialist care is provided under unmanaged traditional fee- for-service insurance, as many have argued it is, substitution of primary care need not adversely affect quality and may improve it.
Figure 4
|
Figure 5
|
Figure 6
|
Figure 7
|
| HMOs | Non-HMOs | Difference | |
| FLU SHOT | 21% | 18% | 3%* |
| MAMMOGRAPHY | 57 | 52 | 5* |
| SMOKING CESSATION ADVICE | 34 | 32 | 2 |
* The difference between HMOs and non-HMOs is statistically significant.
HSC Community Tracking Study Household Survey, 1996-1997
Figure 8
|
Figure 9 |
| HMOs | Non-HMOs | Difference | |
| SATISFACTION (percent very satisfied) With overall care With PCP choice With specialist choice |
58% 65 69 |
63% 69 76 |
-5% -5* -7* |
| RATING OF LAST PHYSICIAN VISIT (percent giving excellent rating) Thoroughness of exam Doctor’s listening Doctor’s explanations |
36 41 42 |
39 44 45 |
-4* -3* -3* |
| PATIENT TRUST IN PHYSICIAN (percent strongly agreeing) Doctor puts medical needs first Doctor will refer when needed Doctor will not perform unnecessary tests |
63 64 68 |
69 71 67 |
-6* -7* 0 |
* The difference between HMOs and non-HMOs is statistically significant.
HSC Community Tracking Study Household Survey, 1996-1997
Implications of the Findings
![]() he study has shown that consumers face a
number of trade-offs when choosing between HMOs and other types of health insurance. HMOs
provide more primary care and preventive services, as well as lower out-of-pocket costs
and fewer financial barriers to care. At the same time, they provide less specialist care
and they raise administrative barriers to care. In addition, patients in HMOs report less
satisfaction, less trust in physicians and lower ratings of physician visits than their
counterparts in other plans. Judgments about the implications of the study’s findings,
some of which are favorable to HMOs and some not, thus depend on individual preferences
and values.
he study has shown that consumers face a
number of trade-offs when choosing between HMOs and other types of health insurance. HMOs
provide more primary care and preventive services, as well as lower out-of-pocket costs
and fewer financial barriers to care. At the same time, they provide less specialist care
and they raise administrative barriers to care. In addition, patients in HMOs report less
satisfaction, less trust in physicians and lower ratings of physician visits than their
counterparts in other plans. Judgments about the implications of the study’s findings,
some of which are favorable to HMOs and some not, thus depend on individual preferences
and values.
The trade-offs identified are relevant to dissatisfied consumers who are part of the managed care backlash, employers anxious to limit health insurance costs and policy makers responding to public dissatisfaction or employer cost concerns. They all may have to accept that the cost savings of managed care cannot come without some sacrifice in nonfinancial barriers to care or even perceived quality. The existence of this trade-off argues for a policy emphasis on ensuring consumer choice, so that individuals may choose the type of insurance they prefer. Policy concern about consumers’ dissatisfaction with HMOs might be lower if consumers had a choice between an HMO and other insurance in the first place. The advantages of offering choice, however, have to be weighed against some important disadvantages, such as higher administrative costs and the potential inefficiencies and inequities arising from favorable or adverse selection among product types.
In any case, choice alone is unlikely to markedly diminish differences in satisfaction. As part of the analysis, we estimated separate HMO effects for the subgroups that did and did not have a choice between an HMO and other types of insurance. Across nearly all measures, including those related to consumer satisfaction, HMO effects did not differ significantly between the two groups. This is not surprising. Consumers may choose HMOs because of lower out- of-pocket cost, easier access to primary care or less paperwork, but nonetheless feel less satisfied with their health care than individuals not in HMOs.
Consumer dissatisfaction with HMOs is important regardless of its cause, because it has combined with provider pressure to become the impetus behind proposals for greater regulation of managed care. The results of this study suggest, however, that public opinion about HMOs should not be the sole basis for designing policy solutions. While the results confirm that HMO enrollees are less satisfied with their health care and less trusting of their physicians, we found negligible differences in reported unmet needs or delayed care. In addition, although we did not measure quality of care, we did not find differences in the amount of three important services received: hospital days, surgeries and emergency room visits. These findings raise the question of whether patient dissatisfaction is based on differences in the actual care received in HMOs, compared with other forms of insurance.
Better understanding of what lies behind consumer dissatisfaction is important if policy is to be based on more than anecdotes and public opinion. In part, this understanding can come from research using data obtained from consumers, such as that reported here, but ultimately information is needed on differences in clinical quality of care between HMOs and other types of insurance.
Regardless of the reasons for their dissatisfaction, consumers’ pressure for less restrictive forms of managed care is likely to constrain the evolution of managed care. For example, proposed federal patient protection legislation would restrict the use of care management tools that are designed to encourage cost-effective use of services, such as limits on access to providers without referrals or some types of financial incentives. Such restrictions will make implementation and improvement of care manage- ment tools more difficult for HMOs. Responding to political pressure from consumers to limit what health plans can do poses a challenge for policy makers. They must balance potential benefits in the form of consumer satisfaction and potential protection of quality against the opportunities for costs savings and potential quality improvement that are lost due to limiting care management tools.
Data Sources and Methodology
![]() his Issue Brief presents findings from
HSC’s Community Tracking Study Household Survey, a nationally representative telephone
survey of the civilian, noninstitutionalized population conducted in 1996 and 1997. Data
were supplemented by in-person interviews of households without telephones to ensure their
proper representation. The overall response rate was 65 percent. This study is based on
data from more than 35,000 nonelderly individuals with private insurance.
his Issue Brief presents findings from
HSC’s Community Tracking Study Household Survey, a nationally representative telephone
survey of the civilian, noninstitutionalized population conducted in 1996 and 1997. Data
were supplemented by in-person interviews of households without telephones to ensure their
proper representation. The overall response rate was 65 percent. This study is based on
data from more than 35,000 nonelderly individuals with private insurance.
The effects of HMOs were calculated using multivariate statistical models that control for differences in the population of people enrolled in HMOs and other types of insurance. The models used an extensive set of control variables, encompassing demographic characteristics, health status, preferences, having a choice between an HMO and other insurance and location in specific local health care markets. These extensive controls reduce the likelihood of bias from unmeasured, confounding variables. Extensive tests indicated that this selection bias did not appear to pose a serious risk to the validity of our analysis.
Vulnerable Subgroups
![]() e tested whether HMO effects were
different for various vulnerable groups (people in poor health, the poor, minorities and
children). The study found no consistent evidence that HMO effects for these groups
differed from its effects for their counterparts in the rest of the population (people in
good health, the nonpoor, whites and adults, respectively). Tests of differences in HMO
effects for subgroups were statistically significant in only a fraction of cases. Because
tests of HMO effects for subgroups are weaker than tests for overall effects for the full
sample, failure to detect subgroup differences in HMOs’ effects does not necessarily mean
they do not exist. Therefore, we also looked for patterns among effects that may not have
met standards of statistical significance.
e tested whether HMO effects were
different for various vulnerable groups (people in poor health, the poor, minorities and
children). The study found no consistent evidence that HMO effects for these groups
differed from its effects for their counterparts in the rest of the population (people in
good health, the nonpoor, whites and adults, respectively). Tests of differences in HMO
effects for subgroups were statistically significant in only a fraction of cases. Because
tests of HMO effects for subgroups are weaker than tests for overall effects for the full
sample, failure to detect subgroup differences in HMOs’ effects does not necessarily mean
they do not exist. Therefore, we also looked for patterns among effects that may not have
met standards of statistical significance.
No strong patterns emerged that would suggest that HMO effects for one group were systematically different from effects for the rest of the population. HMOs significantly reduced Hispanics’ satisfaction and their trust in physicians more than they reduced that of whites, but differences in effects for Hispanics did not extend to other domains. Particular attention has been given to the question of whether HMOs stint on care for persons in poor health. Our results do not substantiate these concerns.
Journal Articles
This Issue Brief is adapted from six articles on "Do HMOs Make a Difference?" from Inquiry, Vol. 36, Issue 4 (Winter 1999/2000).
- "Do HMOs Make a Difference? Introduction" by James D. Reschovsky and Peter Kemper
- "Do HMOs Make a Difference? Data and Methods" by James D. Reschovsky
- "Do HMOs Make a Difference? Access to Health Care" by James D. Reschovsky
- "Do HMOs Make a Difference? Use of Health Services" by Ha T. Tu, Peter Kemper and Holly J. Wong
- "Do HMOs Make a Difference? Consumer Assessments of Health Care" by Timothy Lake
- "Do HMOs Make a Difference? Summary and Implications" by Peter Kemper, James D. Reschovsky and Ha T. Tu
ISSUE BRIEFS are published by the Center for Studying Health System Change.
President: Paul B. Ginsburg
Director of Public Affairs: Ann C. Greiner
Editor: The Stein Group