Who Declines Employer-Sponsored Health Insurance and Is Uninsured?
Issue Brief No. 22
October 1999
Peter J. Cunningham, Elizabeth Schaefer, Christopher Hogan
![]() wenty percent of all uninsured persons are offered health insurance by their employer
or a family member’s employer but choose not to enroll in the offered plan(s). Most
persons who do not "take up" or enroll in available employer-
sponsored coverage cite cost as the main reason why. This Issue Brief, based on two
surveys conducted as part of the Center for Studying Health System Change’s (HSC)
Community Tracking Study, presents new findings on who declines employer-
sponsored coverage and is uninsured as a result. Given the importance of cost in
an individual’s decision whether to enroll in employer-sponsored coverage, policy
makers need to consider ways to address the problem identified by this study:
low take-up rates among lower-income workers.
wenty percent of all uninsured persons are offered health insurance by their employer
or a family member’s employer but choose not to enroll in the offered plan(s). Most
persons who do not "take up" or enroll in available employer-
sponsored coverage cite cost as the main reason why. This Issue Brief, based on two
surveys conducted as part of the Center for Studying Health System Change’s (HSC)
Community Tracking Study, presents new findings on who declines employer-
sponsored coverage and is uninsured as a result. Given the importance of cost in
an individual’s decision whether to enroll in employer-sponsored coverage, policy
makers need to consider ways to address the problem identified by this study:
low take-up rates among lower-income workers.
Insurance Coverage
![]() ore than two-thirds of persons
in the United States under age
65 have access to employer-sponsored health insurance either directly through
their own employers or indirectly as dependents of family members who are offered
insurance by their employer.1
ore than two-thirds of persons
in the United States under age
65 have access to employer-sponsored health insurance either directly through
their own employers or indirectly as dependents of family members who are offered
insurance by their employer.1
Of those with access to employer-sponsored coverage, estimates from HSC’s 1996-1997 Household Survey show that 14 percent are not enrolled (see Figure 1). Most of those not enrolling have other coverage, such as Medicaid or other public coverage (about one-third), or private insurance that was purchased directly or was provided by someone outside the family (another one-third). Only one-third of those who do not enroll in employer-sponsored coverage are uninsured, or 5 percent of all persons with access to employer-sponsored coverage.
Nevertheless, this 5 percent represents 7.3 million uninsured persons, according to the Household Survey, or about 20 percent of all uninsured persons, 2.2 million of whom are children.2
Thus, approximately one in five uninsured persons has access to employer-sponsored coverage, either through his or her own employer or as a dependent of another family member.
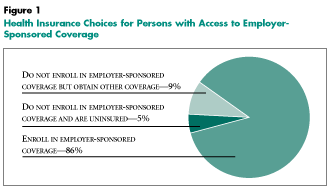
HSC Community Tracking Study, Household Survey, 1996-1997
Enrollment Barriers: Low Income and High Premiums
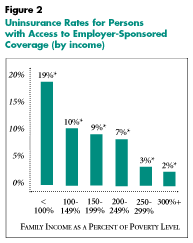
![]() ow-income persons with access to employer-sponsored coverage are much more likely to be uninsured than middle- and upper-income persons. Among those with access and whose family income is below the poverty line, 19 percent are uninsured (see Figure 2).
That figure declines
dramatically as family income increases.
ow-income persons with access to employer-sponsored coverage are much more likely to be uninsured than middle- and upper-income persons. Among those with access and whose family income is below the poverty line, 19 percent are uninsured (see Figure 2).
That figure declines
dramatically as family income increases.
The dramatic difference in uninsurance rates by income suggests that low-income persons are not able to afford the employee share of the premium. Indeed, when asked in the Household Survey why they did not enroll in an employer-sponsored plan that was offered, two-thirds of all uninsured workers and three-fourths of low-income uninsured workers cited cost as the main reason for declining coverage. The remainder declined coverage because of personal preference, such as not needing or wanting insurance, or for some other unspecified reason.
Cost is a barrier to enrollment for low-income workers, not only because employees’ share of premiums consume a higher percentage of their income, but also because the actual cost of health insurance is often higher for low-wage workers than workers with wages that put them in middle- and upper-income brackets. Figure 3 shows findings from the 1997 RWJF Employer Health Insurance Survey on average employee premiums and take-up rates by the typical wage level of the firm. These findings show that employee contributions, even for the least expensive plan offered, tend to be higher in firms that employ primarily low-wage workers. It is not surprising, therefore, that firms with a large number of low-wage workers have significantly lower take-up rates (78 percent) than higher-wage firms.
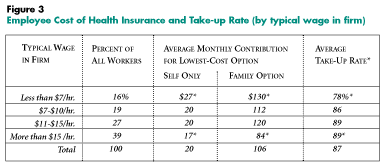
RWJF Employer Health Insurance Survey, 1997
Other Factors Associated with Enrollment Decisions
![]() igh uninsurance among those with access to employer-sponsored coverage is also more prevalent among young adults, racial/ ethnic minorities and persons who are
in poor health.
igh uninsurance among those with access to employer-sponsored coverage is also more prevalent among young adults, racial/ ethnic minorities and persons who are
in poor health.
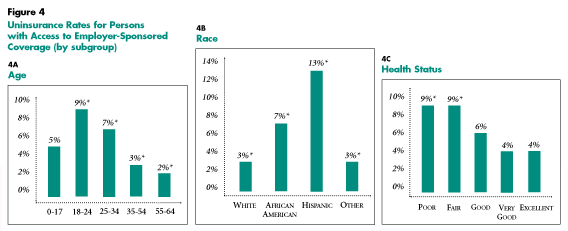
Age. Young adults with access to employer-sponsored insurance have the highest uninsurance rate (9 percent) of all age groups (see Figure 4A). This may reflect both lower incomes and good health among young adults. It also suggests a trade-off between the uncertain benefits of health insurance and spending on other things.
Race. A disproportionately high percentage of African Americans and Hispanics with access to employer-sponsored insurance are uninsured (7 percent and 13 percent, respectively), compared with whites (3 percent). This may be due to lower incomes among African Americans and Hispanics, a greater likelihood of working in jobs where employee contributions for health insurance are higher and/or cultural differences in the perceived importance of health insurance (see Figure 4B).
Health Status. Persons in fair or poor health with access to employer-sponsored coverage are more likely to be uninsured (9 percent each) than those in relatively good health (see Figure 4C). This is surprising given the fact that persons in fair or poor health are more likely to benefit from health insurance, and some may be eligible for public coverage. Higher uninsurance rates among those in fair or poor health reflect in part their generally lower incomes.
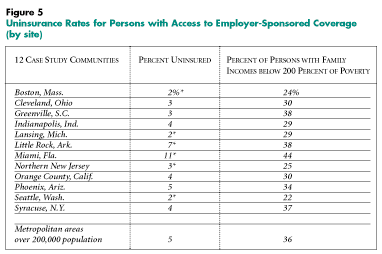
Site. Uninsurance rates among those with access to employer-sponsored coverage vary considerably across HSC’s 12 case study communities, from a high of 11 percent in Miami to a low of 2 percent in Boston, Lansing and Seattle (see Figure 5). As expected, uninsurance rates among those with access to employer-sponsored coverage are highest in communities with the largest number of low-income persons.
HSC Community Tracking Study, Household Survey, 1996-1997
HSC Community Tracking Study, Household Survey, 1996-1997
Policy Implications
![]() mployer-sponsored health insurance
has long been an affordable and attractive way for most individuals to obtain
coverage. Group rates, employer-subsidized premiums and the exclusion from
taxes of the employer’s share of the premium have brought the cost of coverage
within relatively easy reach for most workers. Despite these advantages,
however, past increases in premiums and in the employee share of the premium
have made the cost prohibitively high
for many low-income workers.
mployer-sponsored health insurance
has long been an affordable and attractive way for most individuals to obtain
coverage. Group rates, employer-subsidized premiums and the exclusion from
taxes of the employer’s share of the premium have brought the cost of coverage
within relatively easy reach for most workers. Despite these advantages,
however, past increases in premiums and in the employee share of the premium
have made the cost prohibitively high
for many low-income workers.
A return to large annual increases in health insurance premiums-as some are predicting-could further erode the affordability of employer-sponsored coverage for some workers.
Many also fear that pressure to increase premiums could arise from legislation that would regulate managed care plans-such as patients’ bill of rights legislation-and other health insurance reforms. Given the important role that costs play in a worker’s decision not to enroll in an employer-sponsored plan, large increases in health insurance premiums or increases in the proportion of the premiums that employees pay could result in more employees opting out of coverage, especially lower-income workers.
High employee premium contributions could be a problem for those leaving welfare for work as a result of the 1996 Temporary Assistance for Needy Families legislation. These individuals often face the loss of Medicaid eligibility-many times inappropriately-and frequently are not offered coverage at their workplace. However, even for those former welfare recipients who are offered insurance by their employer, the cost of these plans may be prohibitively high.
What can be done to increase enrollment among the 20 percent of uninsured persons with access to employer-sponsored coverage? Enrolling all or most in employer-sponsored plans that are available to them would do more to decrease the number of uninsured than other incremental expansions that have passed in recent years or that are being considered, including the State Children’s Health Insurance Program and Medicare buy-ins for the near elderly.
Since cost appears to be the major barrier for those who do not enroll in plans, one option is to offer additional financial incentives to enroll, such as extending eligibility of the modest tax subsidies being proposed for persons who do not have access to employer-sponsored coverage to include those that do. Another option, combining subsidies with individual mandates-such as the recent proposal to mandate children’s coverage-could further enhance enrollment among those with access to insurance who, for a variety of reasons, have not enrolled in offered plans. Alternatively, existing public insurance programs such as Medicaid could be expanded to provide a low-cost option to low-income workers who cannot afford the premiums of their employer-sponsored plans.
Any tax subsidy or expansion of public coverage would also have to be available for those low-income persons who are already enrolled in employer-sponsored plans. This would make these policies much more costly and would increase concerns about the "crowding out" or substituting of existing private insurance coverage with publicly provided or subsidized coverage. But this inefficiency in targeting incremental insurance expansions needs to be balanced against the potential public benefit of expanded health insurance for low-income persons who are uninsured, and reducing premium costs for those low-income persons who are enrolled but face a heavy financial burden as a result.
Data Sources
![]() his Issue Brief presents
findings from two surveys that are a part of HSC’s Community Tracking Study.
The Household Survey, conducted in 1996 and 1997, is a nationally representative
telephone survey of the civilian, non-institutionalized population. Data were
supplemented by in-person interviews of households without telephones to ensure
proper representation. The survey contains observations on nearly 33,000 families
and 60,000 individuals. The overall response rate was 65 percent for families.
The 1997 Robert Wood Johnson Foundation Employer Health Insurance Survey is a
nationally representative telephone survey of private and public employers. It
is based on responses of 21,545 establishments. The overall response rate was
60 percent.
his Issue Brief presents
findings from two surveys that are a part of HSC’s Community Tracking Study.
The Household Survey, conducted in 1996 and 1997, is a nationally representative
telephone survey of the civilian, non-institutionalized population. Data were
supplemented by in-person interviews of households without telephones to ensure
proper representation. The survey contains observations on nearly 33,000 families
and 60,000 individuals. The overall response rate was 65 percent for families.
The 1997 Robert Wood Johnson Foundation Employer Health Insurance Survey is a
nationally representative telephone survey of private and public employers. It
is based on responses of 21,545 establishments. The overall response rate was
60 percent.
Notes
1. We assume that all employer offerings include the option for family coverage. The 1997 RWJF Employer Health Insurance Survey indicates that 98 percent of employees who are offered health insurance are offered a family option.
2. These estimates are based on the 1996-1997 Community Tracking Study Household Survey estimate of 35.4 million uninsured persons, which is somewhat lower than the 1996 estimates from the Current Population Survey. For a discussion of the reasons for the differences, see HSC Technical Publication #16.
Related HSC Publications
- Next Steps in Incremental Health Insurance Expansions: Who Is Most Deserving, Issue Brief No. 12, April 1998
- More Small Firms Offer Health Insurance but Fewer Employees Enroll, Data Bulletin No. 10, Winter 1998