Growth of Medicaid-Dominated HMOs
Data Bulletin No. 11
Spring 1998
![]() edicaid enrollment in health maintenance organizations (HMOs) has grown dramatically--from 2.6 million (8 percent of beneficiaries) in 1993 to 7.7 million (23 percent of beneficiaries) in 1996. Nearly half of all enrollees
in 1996 were in Medicaid-dominated plans in which Medicaid beneficiaries comprised at least 75 percent of the total enrollment.
New plans entering the market maintained this same balance, with more than half being Medicaid dominated.
edicaid enrollment in health maintenance organizations (HMOs) has grown dramatically--from 2.6 million (8 percent of beneficiaries) in 1993 to 7.7 million (23 percent of beneficiaries) in 1996. Nearly half of all enrollees
in 1996 were in Medicaid-dominated plans in which Medicaid beneficiaries comprised at least 75 percent of the total enrollment.
New plans entering the market maintained this same balance, with more than half being Medicaid dominated.
CHARACTERISTICS OF MEDICAID-DOMINATED PLANS
![]() n 1996, there were 156 Medicaid-dominated HMOs, which accounted for
48 percent of all plans serving Medicaid.
The Medicaid-dominated plans have several characteristics in common:
n 1996, there were 156 Medicaid-dominated HMOs, which accounted for
48 percent of all plans serving Medicaid.
The Medicaid-dominated plans have several characteristics in common:
- Most of these plans are small; 90 percent have fewer than 50,000 members.
- Most plans that are Medicaid-dominated are basically Medicaid-only: 92 percent
(144 plans) were Medicaid-only in 1996. More than half of the new plans entering
the market between 1993 and 1996 were Medicaid-only plans. (See table on page 2.)
It is not known whether these plans intend to enroll commercial members in the future.
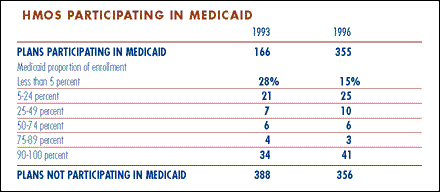
- Plans serving Medicaid tend to be either heavy or light on Medicaid enrollees. Roughly
half of all plans do not participate at all, and of those that do participate,
15 percent had less than 5 percent Medicaid enrollment and 44 percent had 75 percent Medicaid
enrollment or more.
- Medicaid-dominated plans are more likely than other plans to serve the Medicaid disabled population that receives Supplemental Security Income (SSI) benefits. Fifty-eight percent serve SSI versus 45 percent of other Medicaid-serving plans in those states where at least one plan reaches the Medicaid population.
* Medicaid-dominated plans are those in which Medicaid accounts for 75-100 percent of total enrollment.
All other plans that participate in Medicaid are called commercial-based.
CHARACTERISTICS OF PARTICIPATING HEALTH PLANS
![]() ven though there are more small plans, the majority
(54 percent) of Medicaid enrollees in 1996 were in large plans--those with 100,000 or more members and
nearly one-third were in very large plans--those with 250,000 or more members. Enrollees in large plans
were evenly split between independent plans and those affiliated with a major health plan system.
ven though there are more small plans, the majority
(54 percent) of Medicaid enrollees in 1996 were in large plans--those with 100,000 or more members and
nearly one-third were in very large plans--those with 250,000 or more members. Enrollees in large plans
were evenly split between independent plans and those affiliated with a major health plan system.
Commercial health plan participation is relatively widespread across the country, with heavier pockets of participation in the Mid-Atlantic and Pacific states, and lower participation in the South-Central and South- Atlantic regions. (See graph.) Eighty-seven percent of Medicaid enrollees in HMOs live in just 16 states: Arizona, California, Connecticut, Florida, Illinois, Michigan, Minnesota, Missouri, New Jersey, New York, Ohio, Oregon, Pennsylvania, Tennessee, Virginia and Washington. As of June 1996, 15 states had no full-risk plan serving Medicaid.
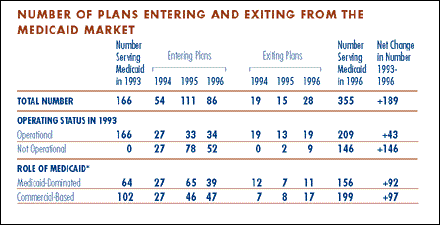
The group of plans that first began serving Medicaid enrollees in 1994 was evenly divided between plans that were operational in 1993 and newly formed plans. But this balance changed dramatically in 1995 and 1996 as newly formed plans began to heavily dominate the mix of plans new to Medicaid.
While the number of plans participating in the Medicaid market more than doubled between 1993 and 1996, 62 plans left the market. There is concern about whether commercial-based plans will pull out of the market as states reduce their capitation rates, but the 1996 data do not show that these plans represent an increasing proportion of plans leaving. Some of the plans that appear to have left may actually still be serving the Medicaid market under another name due to a merger.
IMPLICATIONS FOR POLICYMAKERS
![]() rom a public policy perspective, it is not clear yet whether Medicaid-dominated plans are a positive development.
If traditional safety net providers are more involved in these plans than plans with a broader mix of enrollees,
then they are likely to be better attuned to the needs of Medicaid enrollees. However, the role of safety net
providers in these plans relative to other plans is not yet well understood. Since Medicaid-dominated plans may
not have the resources--or pressure from employers--to deliver all contracted services or to develop state-of-the-art
quality improvement systems, there is a greater burden on state policymakers to monitor their quality of care.
rom a public policy perspective, it is not clear yet whether Medicaid-dominated plans are a positive development.
If traditional safety net providers are more involved in these plans than plans with a broader mix of enrollees,
then they are likely to be better attuned to the needs of Medicaid enrollees. However, the role of safety net
providers in these plans relative to other plans is not yet well understood. Since Medicaid-dominated plans may
not have the resources--or pressure from employers--to deliver all contracted services or to develop state-of-the-art
quality improvement systems, there is a greater burden on state policymakers to monitor their quality of care.
This Data Bulletin is based on data from Health Care Financing Administration Medicaid managed care enrollment reports for June 1993-1996, the Group Health Association of America Directory of HMOs for 1993-1995, the InterStudy directory for 1996 and a list of national and multiregional HMOs with more than 100,000 enrollees developed for the Center for Studying Health System Change. The term HMO is used here to encompass full-risk plans serving Medicaid, regardless of whether they are licensed as HMOs.
This Data Bulletin is adapted from "Changes in Health Plans Serving Medicaid, 1993-1996," by Suzanne Felt-Lisk and Sara Yang, which appeared in the September/October 1997 issue of Health Affairs. The research was conducted by Mathematica Policy Research, Inc., in collaboration with the Center for Studying Health System Change.
