
Data Bulletin No. 13
Fall 1998
![]() he much feared upswing in health care costs has not yet materialized. Based on the most current available data, Health System Change (HSC) finds only a small rise in the rate of increase in costs. For each of the past three years, HSC has reviewed a wide array of data sources to track cost trends and help interpret them for public and private decision makers.
he much feared upswing in health care costs has not yet materialized. Based on the most current available data, Health System Change (HSC) finds only a small rise in the rate of increase in costs. For each of the past three years, HSC has reviewed a wide array of data sources to track cost trends and help interpret them for public and private decision makers.
![]() ne of the key proxies for health care costs is revenues of hospitals, physicians and other providers, based on a per capita basis. According to Milliman and Robertson’s Health Cost Index, which excludes revenues from Medicare patients, these trends declined sharply in the early 1990s, reaching a low of 2.0 percent in 1994. Growth rates have risen since then, but the increases are modest -- a 3.3 percent increase last year, up from 2.1 percent in 1996.
ne of the key proxies for health care costs is revenues of hospitals, physicians and other providers, based on a per capita basis. According to Milliman and Robertson’s Health Cost Index, which excludes revenues from Medicare patients, these trends declined sharply in the early 1990s, reaching a low of 2.0 percent in 1994. Growth rates have risen since then, but the increases are modest -- a 3.3 percent increase last year, up from 2.1 percent in 1996.
Drugs continue to be the fastest growing component of costs, and increases have been in the double digits since 1995. Most of this increase reflects growth in units rather than price. Drug expenditures increased 11.5 percent in 1997, while the drug component of the Consumer Price Index increased only 2.5 percent. The low rates of increase for hospital and physician spending 2.4 percent and 2.0 percent respectively, are in striking contrast.
There are differences in rates of health care cost growth by region, with the highest in the south and the lowest in the west (see bar graph below). These differences presumably relate to the extent or the rate of growth of managed care in a region, but analyzing these relationships is not straightforward.
Bureau of Labor Statistics data on payroll in health services establishments also are useful indicators of trends because they provide the most timely information about health care costs. The increase in payroll expense per capita was 5.3 percent for the first six months of 1998 in relation to the same period in 1997. The increase between 1996 and 1997 was 5.9 percent. These figures belie the notion that the rate of growth of costs is accelerating.
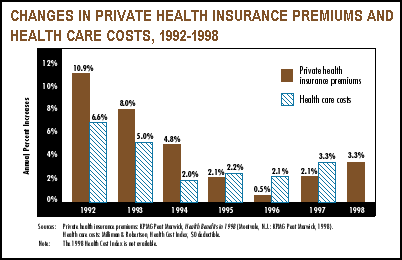
![]() remiums for employment-based health insurance increased only 3.3 percent
this year (see graph on page 1). While this represents an increase over the 2.1 percent rise in 1997, it is far lower than the 5 to 7 percent predictions by industry experts that were reported in the news media. Premium increases were relatively uniform among health plan types, ranging from 2.9 percent for health maintenance organizations (HMOs) and point-of-service (POS) plans to 3.8 percent for preferred provider organizations (PPOs).
remiums for employment-based health insurance increased only 3.3 percent
this year (see graph on page 1). While this represents an increase over the 2.1 percent rise in 1997, it is far lower than the 5 to 7 percent predictions by industry experts that were reported in the news media. Premium increases were relatively uniform among health plan types, ranging from 2.9 percent for health maintenance organizations (HMOs) and point-of-service (POS) plans to 3.8 percent for preferred provider organizations (PPOs).
From 1992 to 1994, premium increases exceeded underlying cost increases by a substantial margin. This started to reverse in 1995, and in 1996 and 1997, premium increases lagged behind the key proxy for costs, provider revenues. Some analysts had expected that 1998 premium trends would be higher than the trends in provider revenues, but with 1998 premium increases no greater than the 1997 provider revenue increases, this is unlikely to occur.
![]() inally, the low rates of cost increases are benefiting consumers. Earlier in the 1990s, when the growth rates of premiums were dropping, the proportion of premiums paid by employees rose substantially. This trend leveled off in 1995 and 1996, and employee contributions have declined since then. Possible factors contributing to this include a delayed reaction on the part of employers to the slowdown in premium growth and tightening labor markets.
inally, the low rates of cost increases are benefiting consumers. Earlier in the 1990s, when the growth rates of premiums were dropping, the proportion of premiums paid by employees rose substantially. This trend leveled off in 1995 and 1996, and employee contributions have declined since then. Possible factors contributing to this include a delayed reaction on the part of employers to the slowdown in premium growth and tightening labor markets.
Another plus for consumers is that out-of-pocket spending for medical services is down substantially -- 9 percent lower in 1995 than in 1990, according to the most recent data from the Department of Labor’s Consumer Expenditure Survey. This may be due to rapid shifts from conventional coverage to managed care plans, where patient cost sharing is much lower.
![]() remium increases could well be higher next year as insurers, experiencing low profit margins, become less aggressive in keeping prices low in order to expand market share. But over the longer term, the underlying cost of health care remains the dominant influence on the direction of premium trends. Factors that could lead to higher increases are the effects of responses to negative sentiment about managed care (e.g., looser controls on utilization) and more provider consolidation. Mitigating these effects are the continuing excess capacity among health providers and the single-mindedness of purchasers to hold their costs down.
remium increases could well be higher next year as insurers, experiencing low profit margins, become less aggressive in keeping prices low in order to expand market share. But over the longer term, the underlying cost of health care remains the dominant influence on the direction of premium trends. Factors that could lead to higher increases are the effects of responses to negative sentiment about managed care (e.g., looser controls on utilization) and more provider consolidation. Mitigating these effects are the continuing excess capacity among health providers and the single-mindedness of purchasers to hold their costs down.
This Data Bulletin is adapted from "Tracking Health Care Costs: What’s New In 1998?," by Paul B. Ginsburg and Jon R. Gabel, which appeared in the September/October 1998 issue of Health Affairs.