
How Widespread Is Managed Competition?
Data Bulletin No. 12
Summer 1998
Stephen H. Long, M. Susan Marquis
![]() he managed competition strategy -- the framework that was popularized by Alain Enthoven -- seeks to stimulate price and quality competition among insurers vying for consumers.1 Many policy makers hope that the private sector will promote managed competition in order to achieve these objectives. However, recent findings from the 1997 Robert Wood Johnson Foundation (RWJF) Employer Health Insurance Survey reveal that few private employers offer employees a choice of plans, give employees financial incentives to choose economical plans or provide information so that employees can evaluate the quality of care they receive - the three hallmarks of managed competition.
he managed competition strategy -- the framework that was popularized by Alain Enthoven -- seeks to stimulate price and quality competition among insurers vying for consumers.1 Many policy makers hope that the private sector will promote managed competition in order to achieve these objectives. However, recent findings from the 1997 Robert Wood Johnson Foundation (RWJF) Employer Health Insurance Survey reveal that few private employers offer employees a choice of plans, give employees financial incentives to choose economical plans or provide information so that employees can evaluate the quality of care they receive - the three hallmarks of managed competition.
LIMITED CHOICE
![]() verall, only 17 percent of private employers that offer insurance to their employees provide a choice among plans. Even though large groups are more likely than small ones to offer choice, only one-third of establishments of firms with 100 or more employees offer a choice of plans. Counting employees rather than employers, still less than half -- 41 percent -- who are offered insurance can choose among two or more plans.
verall, only 17 percent of private employers that offer insurance to their employees provide a choice among plans. Even though large groups are more likely than small ones to offer choice, only one-third of establishments of firms with 100 or more employees offer a choice of plans. Counting employees rather than employers, still less than half -- 41 percent -- who are offered insurance can choose among two or more plans.
HIGH-PRICED PLANS SUBSIDIZED
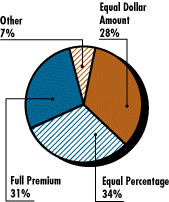
![]() nly about 27 percent of employees in firms offering a choice of plan face financial incentives to shop for the lower-priced plans, because most employers subsidize the difference in the price of plans by contributing more for the higher-priced plans. Specifically, 31 percent of employers pay the full cost of employee-only coverage regardless of the plan selected; 34 percent of employers pay the same share of the plan cost and 28 percent pay equal dollar amounts regardless of its magnitude (see pie chart on financial incentives).
nly about 27 percent of employees in firms offering a choice of plan face financial incentives to shop for the lower-priced plans, because most employers subsidize the difference in the price of plans by contributing more for the higher-priced plans. Specifically, 31 percent of employers pay the full cost of employee-only coverage regardless of the plan selected; 34 percent of employers pay the same share of the plan cost and 28 percent pay equal dollar amounts regardless of its magnitude (see pie chart on financial incentives).
Employers have shown little movement toward the equal dollar contributory policy prescribed by managed competition. Only 4 percent of employers that subsidized the difference in premium among plans in 1996 switched to an equal dollar contribution policy in 1997.
Employer Provision
|
Provision of Comparative Quality |
 |
 |
|
|
|
CONSUMER INFORMATION SPARSE
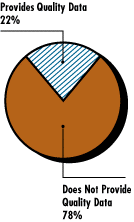
![]() fforts have been made in the public and private sectors to develop measures to help consumers compare plans on the basis of quality and other indicators of plan performance. However, the provision of information is not widespread. Of those offering choice, only about one-quarter of the largest establishments -- with 500 or more employees -- provide results beyond basic plan descriptions, including patient satisfaction results, NCQA’s Health Plan Employer Data and Information Set (HEDIS) measures or other comparative data about plans (see pie chart on quality data).
fforts have been made in the public and private sectors to develop measures to help consumers compare plans on the basis of quality and other indicators of plan performance. However, the provision of information is not widespread. Of those offering choice, only about one-quarter of the largest establishments -- with 500 or more employees -- provide results beyond basic plan descriptions, including patient satisfaction results, NCQA’s Health Plan Employer Data and Information Set (HEDIS) measures or other comparative data about plans (see pie chart on quality data).
IMPLICATIONS FOR MANAGED COMPETITION
![]() any policy makers and business leaders have embraced the principles of managed competition as a means to achieve affordable, quality health care and contain growth in health care spending. However, managed competition has not yet been fully implemented by most employers, even among large firms. Proposed consumer protection legislation in Congress could change this on the information front. But for now, employers rather than employees appear to be driving health plan choice, and the consumer-driven competitive system envisioned under managed competition has not yet been achieved.
any policy makers and business leaders have embraced the principles of managed competition as a means to achieve affordable, quality health care and contain growth in health care spending. However, managed competition has not yet been fully implemented by most employers, even among large firms. Proposed consumer protection legislation in Congress could change this on the information front. But for now, employers rather than employees appear to be driving health plan choice, and the consumer-driven competitive system envisioned under managed competition has not yet been achieved.
Note
1. Alain Enthoven and Richard Kronick. “A Consumer Choice Health Plan for the 1990s.”
New England Journal of Medicine, 1989, 320: 29-37, 94-101.
This Data Bulletin presents results from the 1997 Robert Wood Johnson Foundation Employer Health Insurance Survey, a nationally representative telephone survey of private and public employers. It is based on responses of 21,543 private establishments. The survey is a component of Health System Change’s (HSC’s) Community Tracking Study. It was conducted by Research Triangle Institute (RTI) and designed by RAND and RTI, with collaboration from HSC.