
Community Report No. 12
Spring 1999
Cara S. Lesser, Daniel S. Gaylin, Amy M. Andersen, Lawrence D. Brown
![]() n February 1999, a team of researchers visited northern New Jersey to study that community’s health system, how it is changing and the impact of those changes on consumers. More than 60 leaders in the health care market were interviewed as part of the Community Tracking Study by the Center for Studying Health System Change (HSC) and The Lewin Group. Northern New Jersey is one of 12 communities tracked by HSC every two years through site visits and surveys. Individual community reports are published for each round of site visits. The first site visit to northern New Jersey, in April 1997, provided baseline information against which changes are being tracked. The northern New Jersey market studied is defined by the Newark primary metropolitan statistical area (PMSA) and includes Sussex, Warren, Morris, Essex and Union counties.
n February 1999, a team of researchers visited northern New Jersey to study that community’s health system, how it is changing and the impact of those changes on consumers. More than 60 leaders in the health care market were interviewed as part of the Community Tracking Study by the Center for Studying Health System Change (HSC) and The Lewin Group. Northern New Jersey is one of 12 communities tracked by HSC every two years through site visits and surveys. Individual community reports are published for each round of site visits. The first site visit to northern New Jersey, in April 1997, provided baseline information against which changes are being tracked. The northern New Jersey market studied is defined by the Newark primary metropolitan statistical area (PMSA) and includes Sussex, Warren, Morris, Essex and Union counties.
![]() t the time of HSC’s 1997 site visit, hospitals in northern New Jersey had recently undergone extensive consolidation in response to hospital rate deregulation and expected managed care growth. The subsequent closure of one inner city hospital triggered concerns that services would become concentrated in the suburbs and access to care in the inner city would deteriorate. Since then, hospital merger activity has slowed. Dire predictions concerning access to care in the inner city and the viability of the local safety net have not materialized, although some downsizing has occurred. Meanwhile, health plan consolidation has proceeded swiftly due to national and local mergers.
t the time of HSC’s 1997 site visit, hospitals in northern New Jersey had recently undergone extensive consolidation in response to hospital rate deregulation and expected managed care growth. The subsequent closure of one inner city hospital triggered concerns that services would become concentrated in the suburbs and access to care in the inner city would deteriorate. Since then, hospital merger activity has slowed. Dire predictions concerning access to care in the inner city and the viability of the local safety net have not materialized, although some downsizing has occurred. Meanwhile, health plan consolidation has proceeded swiftly due to national and local mergers.
Other key developments since 1997 include:
- Diverse Market with Local and Regional Influences
- Turmoil in the Health Plan Market
- Consolidation and Financial Woes
- Physician-Hospital Contracting Entities Off to Slow Start
- Safety Net Providers Adapt to Changing
- Issues to Track
- Northern New Jersey Compared to Other Communities HSC Tracks
- Background and Observations
![]() he northern New Jersey market, as defined by the Newark PMSA, spans a diverse area, including a number of inner cities, affluent suburbs and rural communities. It is noted for its high concentration of both wealth and poverty and significant ethnic and racial disparities. Health status is also highly variable; rates of AIDS and substance abuse in the city of Newark are among the nation’s highest.
he northern New Jersey market, as defined by the Newark PMSA, spans a diverse area, including a number of inner cities, affluent suburbs and rural communities. It is noted for its high concentration of both wealth and poverty and significant ethnic and racial disparities. Health status is also highly variable; rates of AIDS and substance abuse in the city of Newark are among the nation’s highest.
The area’s urban-suburban split segments the hospital market, with some systems squarely anchored in the suburbs and others operating almost entirely in the inner cities. In contrast, health plans typically operate on a statewide or regional basis, with broad provider networks to accommodate the area’s large employers and many commuters to and from nearby New York, Pennsylvania and Delaware. With unemployment at only 4.8 percent, employers offer generous, nonrestrictive health benefits to attract workers. Health maintenance organization (HMO) penetration remains low (just 24 percent, compared with an average of 34 percent for metropolitan areas), and organized activity by purchasers is minimal.
State policy has played an important role in shaping the health care market in northern New Jersey, although its focus has changed in recent years. In the early 1990s, the state began to deregulate the hospital industry. Hospital rate setting was abolished, a process for relaxing and streamlining certificate of need (CON) regulations was initiated and the state program for reimbursing hospitals for charity care was restructured and scaled back. Since then, the state has continued efforts to expand access to insurance, building on small-group and individual insurance market reforms passed in 1992. Premium subsidies for the working poor were enacted in 1995, and a new children’s health insurance program, NJKidCare, was established in April 1998.
Like many other states, New Jersey has turned its attention to regulating managed care and has been particularly aggressive in this regard. The broad-ranging Health Care Quality Act (HCQA), signed into law in August 1997, contains provisions for consumer protections and a health plan report card that documents patient satisfaction and health plan performance on a variety of clinical measures.
![]() he collapse of two health plans has shaken the northern New Jersey market. Questionable financial arrangements and poor management allegedly led to the failures of both HIP of New Jersey, a prominent group-model HMO, and American Preferred Provider Plan (APPP), a relatively new plan that mainly served the Medicaid market.
he collapse of two health plans has shaken the northern New Jersey market. Questionable financial arrangements and poor management allegedly led to the failures of both HIP of New Jersey, a prominent group-model HMO, and American Preferred Provider Plan (APPP), a relatively new plan that mainly served the Medicaid market.
Following several years of heavy losses, HIP was in desperate financial shape by 1997. HIP sold its physician practices and clinics to PHP Healthcare, a Virginia-based national health care management company, and subcontracted with PHP to provide physician services to its enrollees. The state approved the deal, even though PHP was heavily in debt and was operating at a loss. Although PHP’s financial condition worsened and became more visible, the state contended that it had little regulatory authority to intervene because the arrangement was a subcontract and PHP was based outside of thestate. When PHP subsequently went bankrupt, the state took over HIP’s operations and ultimately moved to dissolve it.
The demise of APPP began when its owner diverted plan funds to two affiliated businesses that subsequently defaulted on the loans. When APPP’s net worth fell below state solvency requirements, the state assumed control of the health plan and filed for bankruptcy on its behalf.
After each collapse, the state took measures to ensure continuity of care and facilitate the transfer of enrollees to other plans. These actions appear to have been largely successful. In the case of APPP, the state was able to transfer all 32,000 Medicaid enrollees to another plan. HIP’s liquidation caused greater displacement, requiring more than 100,000 consumers including an estimated 22,000 Medicaid beneficiaries to find a new health plan. The state mandated a 30-day open enrollment period during which all plans were required to offer coverage at their usual rates. However, these rates were frequently higher than what consumers had paid before, and by the last week of the open enrollment period, an estimated 30,000 HIP members had not selected another plan. In addition, the closure of HIP’s clinics resulted in physician and staff layoffs and some inherent disruptions in continuity of care.
The plans’ failures also have had serious financial repercussions for providers, with estimates of debts of $80-$120 million in the case of HIP and more than $37 million in the case of APPP. Under recent settlements, hospitals and physicians will receive 30 cents on the dollar for all unpaid HIP claims for services prior to the state takeover and 20 to 23 cents on the dollar for unpaid APPP claims that preceded its takeover.
The collapse of HIP and APPP has raised concerns about the state’s regulatory role. Health plan solvency requirements were raised in 1997, but the state is now taking steps to increase its regulatory oversight to prevent similar failures. In addition, legislative proposals, backed by the governor, would create a guaranty fund to help bail out financially troubled plans and to ensure provider payment in the event of a future crisis. Health plans would be required to contribute to this fund, though the New Jersey Association of Health Plans is vigorously opposing the idea, arguing that it constitutes a tax and would increase premiums.
![]() apid consolidation among hospitals was observed during HSC’s 1997 site visit, and today this trend is seen most strikingly among health plans. Much of this is attributed to mergers among national plans, although the local Blue Cross Blue Shield plan’s aggressive acquisition strategy also has played a role.
apid consolidation among hospitals was observed during HSC’s 1997 site visit, and today this trend is seen most strikingly among health plans. Much of this is attributed to mergers among national plans, although the local Blue Cross Blue Shield plan’s aggressive acquisition strategy also has played a role.
The most conspicuous and widely noted consolidation has been led by Aetna Inc., which, with more than one-third of HMO enrollees in northern New Jersey, is the largest HMO in the area. Its market share has grown substantially as a result of its 1997 merger with U.S. Healthcare and its subsequent acquisition of NYLCare in 1998. It stands to increase its market power even more with the recent federal approval of its acquisition of Prudential. Some providers and consumer groups fear that the resulting entity will command tremendous market leverage, reducing payments to providers, raising premiums and diminishing choice.
Meanwhile, Blue Cross Blue Shield of New Jersey has sought to reposition itself after state regulators blocked its proposed merger with Anthem, Inc., a multiregional Blues plan. Among other changes, the plan recently changed its name to Horizon Blue Cross Blue Shield of New Jersey to facilitate its entry into surrounding markets in Delaware and New York under the name Horizon. This allows it to distinguish itself from other Blues plans that are licensed to sell branded products in those regions.
In general, health plans in this market, like their counterparts nationally, have confronted diminishing profit margins in recent years. After several years of holding down premiums to expand market share, plans are seeking increases of 10 percent or more in contracts negotiated in 1999.
In the hospital sector, the merger frenzy appears to have dissipated. In 1997, three major consolidations were underway, largely in response to regulatory change and expected managed care growth. Since then, these systems have continued to reconfigure through additional mergers or merger attempts; in one case, an existing partnership dissolved.
In a worsening financial environment, the two remaining merged systems, St. Barnabas and Atlantic, have struggled with poor financial performance. Although both systems have made strides toward administrative consolidation, there has been little consolidation of clinical services or capacity. Investments in infrastructure to coordinate functions at the system level also have exacted a cost. Moreover, the systems’ financial performance has been strained by assuming the debt load and excess capacity of financially weak hospitals.
Statewide, hospitals’ financial health has been eroding. According to the New Jersey Hospital Association, operating margins have decreased from 1.4 percent in 1996 to -1.3 percent in 1998. Hospitals attribute this decline to a variety of factors, including shortfalls in charity care funding from the state, financial repercussions of health plan failures and continuing payer demand for discounts. The federal Balanced Budget Act (BBA) of 1997 also has played a role, and downward pressure on hospital revenue is expected to intensify as the Act’s remaining provisions are implemented. Hospitals have pressed the state for relief through increased charity care funding and stricter oversight of health plans to ensure timely and adequate payment. The state recently established a task force to determine other measures that may be necessary to strengthen hospitals’ financial status.
![]() ne of the major objectives of the hospital systems formed in the past few years was to improve their bargaining position for managed care contracts. To this end, St. Barnabas and Atlantic each pursued strategies to coordinate contracting across the systems’ hospitals and affiliated physicians. While each appears to have produced modest gains for the hospital partners, both faced setbacks to their physician integration efforts and have begun to revamp their strategies accordingly.
ne of the major objectives of the hospital systems formed in the past few years was to improve their bargaining position for managed care contracts. To this end, St. Barnabas and Atlantic each pursued strategies to coordinate contracting across the systems’ hospitals and affiliated physicians. While each appears to have produced modest gains for the hospital partners, both faced setbacks to their physician integration efforts and have begun to revamp their strategies accordingly.
In January 1997, Atlantic launched a large-scale management services organization (MSO), Health Resource Partners (HRP), to handle managed care risk contracting for nearly 800 affiliated physicians across the four-hospital system. Atlantic invested $12 million in setting up HRP and building the infrastructure necessary to manage risk. However, it was unsuccessful in negotiating acceptable contract terms with plans because of plans’ reluctance to delegate responsibility for clinical care management along with financial risk. The hospital system now has scaled back HRP to provide services for a physician organization associated with just one hospital.
St. Barnabas originally sought to build its network by purchasing physician practices, but, consistent with national trends, it has moved away from this strategy, which yielded fewer benefits than expected. It is currently developing the St. Barnabas Physician Partnership, a super physician-hospital organization (PHO), to coordinate contracting across all of the system’s hospitals and affiliated physicians. At the time of the 1999 site visit, several hundred physicians had submitted applications to join, and the system is targeting more than 4,000 physicians. The partnership has been selected for a Medicare demonstration project to pilot the use of global payment at three hospitals, giving it an important large initial contract. Market observers note that this contract may help St. Barnabas’s PHO to secure the scale needed to change the dynamics of local managed care contract negotiations.
Aside from these initiatives, physician organization remains quite limited in northern New Jersey. Most physicians continue to practice in solo or small-group practices. While there are many PHOs at local hospitals, they do not require physician exclusivity, so they wield little market power.
![]() n 1997, many respondents reported that the northern New Jersey safety net was in peril, largely because of state policy changes with regard to deregulation of hospital rates and the adoption of mandatory Medicaid managed care. Both were expected to exert downward pressure on hospital payment, which many feared would threaten the financial viability of inner city hospitals in particular and diminish access to services for people living in urban areas.
n 1997, many respondents reported that the northern New Jersey safety net was in peril, largely because of state policy changes with regard to deregulation of hospital rates and the adoption of mandatory Medicaid managed care. Both were expected to exert downward pressure on hospital payment, which many feared would threaten the financial viability of inner city hospitals in particular and diminish access to services for people living in urban areas.
Since then, providers’ financial environment overall has worsened, and there has been some downsizing among safety net providers. However, the safety net, by and large, has not deteriorated to the extent anticipated, though serious financial pressures remain.
The state scaled back funding for charity care with the implementation of hospital rate deregulation in 1992, resulting in a dramatic drop from $700 million that year to $500 million in 1993. Funding levels continued to decline steadily for several years, reaching a low of $300 million in 1997. In 1998 and 1999, however, the state increased charity care funding to $320 million annually. The state also increased funding under the Hospital Relief Fund, which targets hospitals with a disproportionate share of high-cost cases, such as HIV/AIDS, tuberculosis and complex neonatal care. An additional $58 million was allocated under this fund in 1998, bringing it up to $183 million in total.
Recent increases in public subsidies for charity care have helped hospitals to hold their ground and have especially benefited inner city hospitals, where much of this care is concentrated. Nevertheless, hospitals’ provision of charity care continues to exceed state funding, and inner city hospitals in particular continue to shoulder significant financial burdens related to uncompensated care.
Some inner city hospitals have pursued strategies that appear to have helped mitigate this financial pressure. For instance, Newark Beth Israel, an inner city tertiary care provider now part of the St. Barnabas system, appears to have been bolstered by its affiliation with financially stronger hospitals. Others have taken advantage of NJKidCare to secure reimbursement for previously uninsured patients. For example, one major local safety net provider, University Health System, noted its efforts to enroll eligible children on site to capture this revenue. Overall, however, slow enrollment in NJKidCare has limited the gains from this program.
Providers also have had to adapt to mandatory Medicaid managed care, which has been phased in rapidly since it was launched in 1995. The program now covers 95 percent of Medicaid beneficiaries eligible through the state’s welfare program and is generating an estimated savings of $400 million a year. Moreover, the low auto-assignment rate relative to other states is considered by many to be a marker of the program’s success in minimizing the potential negative impact on enrollees.
However, Medicaid managed care has produced financial strain for some safety net providers, particularly as the number of uninsured reportedly is growing. Community health centers (CHCs) report declines in revenue, largely due to reduced payment under capitation and reported increases in uncompensated care. As a result, several CHCs have closed sites, reduced hours and staff and scaled back outreach and education programs.
![]() he northern New Jersey health care market continues to experience significant change. While consolidation continues in both sectors, albeit more slowly for hospitals, the financial performance of hospitals and many health plans has worsened considerably. Hospitals are seeking additional state funding for some relief, while plans are looking to employers to increase premiums and, in some cases, relying on state bailouts. Meanwhile, local physicians, still largely unorganized, have secured little bargaining power in the market. At the same time, the safety net did not deteriorate as feared two years ago but remains financially strained.
he northern New Jersey health care market continues to experience significant change. While consolidation continues in both sectors, albeit more slowly for hospitals, the financial performance of hospitals and many health plans has worsened considerably. Hospitals are seeking additional state funding for some relief, while plans are looking to employers to increase premiums and, in some cases, relying on state bailouts. Meanwhile, local physicians, still largely unorganized, have secured little bargaining power in the market. At the same time, the safety net did not deteriorate as feared two years ago but remains financially strained.
As the market continues to change, several key issues warrant tracking:
Northern New Jersey, the highest and lowest HSC study sites and metropolitan areas with over 200,000 population

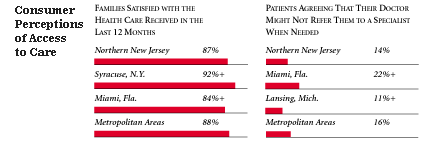

The information in these graphs comes from the Household, Physician and Employer
Surveys conducted in 1996 and 1997 as part of HSC’s Community Tracking Study. The
margins of error depend on the community and survey question and include +/- 2
percent to +/- 5 percent for the Household Survey, +/-3 percent to +/-9 percent
for the Physician Survey and +/-4 percent to +/-8 percent for the Employer Survey.

+ Site value is significantly different from the mean for metropolitan
areas over 200,000 population.
| Northern New Jersey | Metropolitan areas above 200,000 population |
| Population, 19971 | |
| 1,943,494 | |
| Population Change, 1990-19971 | |
| 1.4% | 6.7% |
| Median Income2 | |
| $29,355 | $26,646 |
| Persons Living in Poverty2 | |
| 10% | 15% |
| Persons Age 65 or Older2 | |
| 14% | 12% |
| Persons with No Health Insurance2 | |
| 9.8% | 14% |
|
Sources: 1. U.S. Census, 1997 2. Household Survey Community Tracking Study, 1996-1997 | |

The collapse of two health plans has shaken the northern New Jersey market.
Hospitals’ financial health has been eroding, and they are pressing the state for relief through increased charity care funding and stricter over- sight of payment from health plans.
Most physicians continue to practice in solo or small- group practices. While there are many PHOs, they do not require physician exclusivity, so they wield little market power.
The safety net has not deteriorated to the extent anticipated, though serious financial pressures remain.
The Community Tracking Study, the major effort of HSC, tracks changes in the health system in 60 sites that are representative of the nation. Every two years, HSC conducts surveys in all 60 communities and site visits in the following 12 communities: