
Community Report No. 07
Winter 1999
Jon B. Christianson, Terry West, Melanie L.E. Barraclough
![]() n November 1998, a team of researchers visited Indianapolis, Ind., to study that
community’s health system, how
it is changing and the impact of those changes on consumers. More than 40 leaders in
the health care market were interviewed as part of the Community Tracking Study by
the Center for Studying Health System Change (HSC) and The Lewin Group. Indianapolis
is one of 12 communities tracked by HSC every two years through site visits and
surveys. Individual community reports are published for each round of site visits.
The first site visit to Indianapolis, in November 1996, provided baseline information
against which changes are being tracked. The Indianapolis market encompasses a nine-county
region.
n November 1998, a team of researchers visited Indianapolis, Ind., to study that
community’s health system, how
it is changing and the impact of those changes on consumers. More than 40 leaders in
the health care market were interviewed as part of the Community Tracking Study by
the Center for Studying Health System Change (HSC) and The Lewin Group. Indianapolis
is one of 12 communities tracked by HSC every two years through site visits and
surveys. Individual community reports are published for each round of site visits.
The first site visit to Indianapolis, in November 1996, provided baseline information
against which changes are being tracked. The Indianapolis market encompasses a nine-county
region.
![]() n 1996, five hospital-based systems
dominated the Indianapolis market. These systems, all not-for-profit, owned the
market’s most successful health plans. In addition, they owned or contracted with
most of
the area’s primary care practices. Managed care enrollment was limited. Employers
and state and local policy makers were not active in the health care arena.
With the 1997 merger of two systems, providers in Indianapolis have solidified
their position, and the health plans they own continue to be the most
successful ones in the market. Among the developing market trends:
n 1996, five hospital-based systems
dominated the Indianapolis market. These systems, all not-for-profit, owned the
market’s most successful health plans. In addition, they owned or contracted with
most of
the area’s primary care practices. Managed care enrollment was limited. Employers
and state and local policy makers were not active in the health care arena.
With the 1997 merger of two systems, providers in Indianapolis have solidified
their position, and the health plans they own continue to be the most
successful ones in the market. Among the developing market trends:
- Provider Systems’ Influence Grows Stronger
- Physicians Realign
- Provider-Sponsored Health Plans Maintain Strong Market Position
- PHOs Become Less Important in Contacting Strategies
- Employer Roundtable Takes a Closer Look at Health Plans
- Legislature Pursues More Aggressive Managed Care Policy Agenda
- New Programs for the Uninsured
- Issues to Track
- Indianapolis Compared to Other Communities HSC Tracks
- Background and Observations
![]() everal hospital-based systems have
enhanced their already strong market positions during the past two years, in part to
increase their bargaining leverage with health plans and stimulate revenue growth.
Most significant, Methodist Hospital of Indiana and the Indiana University Medical
Center (with its
affiliate, Riley Hospital for Children) merged in 1997 to create Clarian Health
Partners. This new entity has 1,400 acute care beds - 23 percent of all acute care
beds in the Indianapolis market.
everal hospital-based systems have
enhanced their already strong market positions during the past two years, in part to
increase their bargaining leverage with health plans and stimulate revenue growth.
Most significant, Methodist Hospital of Indiana and the Indiana University Medical
Center (with its
affiliate, Riley Hospital for Children) merged in 1997 to create Clarian Health
Partners. This new entity has 1,400 acute care beds - 23 percent of all acute care
beds in the Indianapolis market.
In the three months immediately following the creation of Clarian, the two partners combined many administrative functions. Respondents reported that the post-merger integration of medical groups has proved difficult and will take time to accomplish. In some specialties, the academic culture of the medical school faculty has apparently clashed with the more entrepreneurial culture of Methodist physicians.
The Methodist-University union ignited some controversy. Competing care systems expressed concern about the potential market power of the merged entity, while community advocacy groups raised issues about the possible impact on the poor and uninsured. Publicly owned Wishard Hospital is closely affiliated with the University’s medical school faculty and is the major provider of indigent care in Indianapolis. The merger raised questions about the future of this relationship and about the continued viability of Wishard as a service provider for the poor and uninsured. In addition, other observers feared that the merger would result in restricted access to care at Riley Hospital, which was widely viewed as a unique and valuable state resource for the treatment of children.
Since the merger, other provider systems in Indianapolis have launched several strategic initiatives in response to these changing market conditions.
![]() recent spate of consolidations among
specialty practices has strengthened the position of some specialists in bargaining
with health plans and provider systems. Although specialists in Indianapolis are
realigning much more actively than they were in 1996, it is not possible to detect
clear trends at this time or to identify common catalysts for change.
recent spate of consolidations among
specialty practices has strengthened the position of some specialists in bargaining
with health plans and provider systems. Although specialists in Indianapolis are
realigning much more actively than they were in 1996, it is not possible to detect
clear trends at this time or to identify common catalysts for change.
In 1996, the Indianapolis metropolitan statistical area (MSA) had 32 percent more specialists per capita than the national average. Today, small, single-specialty practices remain the norm. Typically, specialists still access patients through direct contracts with managed care plans, under fee schedules that have eroded over time or through subcontracts with PHOs. Fees typically are set as a percentage of Medicare reimbursement; few multispecialty groups are available to accept capitated contracts.
In a merger that has drawn considerable local attention, the market’s two largest cardiology groups combined in January 1999. The new organization, Care Group, includes 87 cardiologists, six related subspecialists and 52 primary care physicians. It is the largest cardiology group in the state and, reportedly, one of the largest in the country. Similarly, Community Hospitals’ radiology group has merged with the radiology group at St. Vincent’s and is considering another merger with St. Francis’s group to form a single organization that can serve all three systems. Other recent single- specialty mergers in the market were noted in sports medicine, neurology, urology and orthopedics.
In contrast to the single-specialty approach, SpecPrime is a 350-physician, multispecialty network affiliated with Community Hospitals. SpecPrime contracts with a number of health maintenance organizations (HMOs), including Maxicare, HealthSource and HealthPoint, on a capitated, full-risk basis. It is currently adding specialists and expanding into adjacent geographic areas. Most market observers view SpecPrime’s approach as an exception in the current market for specialty care and do not see it as indicating a trend.
Changes in the organization of physicians have had little impact on Indianapolis’s primary care physician practices, most of which continue to be owned by provider systems or health plans, or remain closely affiliated with provider systems. However, many of the systems and plans that made aggressive efforts to acquire primary care physician practices in the early 1990s are now questioning the wisdom of this strategy. For example, Anthem Blue Cross and Blue Shield, the Blue Cross-Blue Shield plan in Indianapolis, recently sold its 250-member primary care physician arm, the American Health Network, back to member physicians. The network remains in place under physician ownership to represent its physician members in contracting with health plans.
![]() ealth plans owned by local provider
systems, which dominated the market in 1996, have gained even more strength in
Indianapolis. This stands in contrast to other parts of the country, where many
provider-owned plans have struggled.
In general, Indianapolis’s provider-owned plans offering HMO and preferred provider
organization (PPO) products have fared well financially during the
past two years, while other plans, such as those owned by Anthem and Maxicare, have
experienced financial losses. PPO products continue to dominate the
market, although commercial HMO enrollment has grown from 19 percent
at the time of the first site visit to 23
percent in 1997. Between 1996 and 1998, Medicaid managed care penetration grew from
35 to 41 percent in the Indianapolis MSA, while Medicare risk plan enrollment remained
small, increasing from
4 to just 6 percent.
ealth plans owned by local provider
systems, which dominated the market in 1996, have gained even more strength in
Indianapolis. This stands in contrast to other parts of the country, where many
provider-owned plans have struggled.
In general, Indianapolis’s provider-owned plans offering HMO and preferred provider
organization (PPO) products have fared well financially during the
past two years, while other plans, such as those owned by Anthem and Maxicare, have
experienced financial losses. PPO products continue to dominate the
market, although commercial HMO enrollment has grown from 19 percent
at the time of the first site visit to 23
percent in 1997. Between 1996 and 1998, Medicaid managed care penetration grew from
35 to 41 percent in the Indianapolis MSA, while Medicare risk plan enrollment remained
small, increasing from
4 to just 6 percent.
M-Plan, which is owned by Clarian, has the largest share of HMO enrollment; its membership grew from 122,000 in 1996 to 175,000 in 1998. During the same period, Anthem lost approximately the same level of enrollment from both its PPO and HMO products. Many respondents attribute this erosion to Anthem’s lack of attention to the local market as it pursued regional and national expansion strategies.
M-Plan is now attempting to strengthen its statewide presence through a merger with HealthPoint, another provider-owned managed care plan. If completed, this merger would create a 600,000-member plan and a statewide network, with two-thirds of plan members located outside Indianapolis and enrolled in a PPO product.
With the exception of Maxicare, which has 81,000 commercial and Medicaid enrollees, national, for-profit plans continue to play a relatively small role in the Indianapolis market. However, CIGNA recently entered the market through its purchase of HealthSource Indiana, an HMO that serves enrollees statewide. Its ability to grow market share locally remains to be seen.
![]() roviders in the Indianapolis market
are increasingly resistant to assuming financial risk from contracting health plans,
and, as a result, they are lessening their reliance on PHOs as contracting vehicles.
In 1996, provider systems often used their affiliated PHOs to secure full-risk,
globally capitated contracts with health plans. At that time, hospitals and
physicians believed that they could control their costs and realize profits
under global capitation.
roviders in the Indianapolis market
are increasingly resistant to assuming financial risk from contracting health plans,
and, as a result, they are lessening their reliance on PHOs as contracting vehicles.
In 1996, provider systems often used their affiliated PHOs to secure full-risk,
globally capitated contracts with health plans. At that time, hospitals and
physicians believed that they could control their costs and realize profits
under global capitation.
Providers are now reassessing that assumption. Many are insisting that high-cost, difficult-to-control components such as pharmaceuticals be carved out of capitation payments, and that health plans retain some level of financial risk. Furthermore, many physicians are bypassing the PHOs and contracting independently with health plans to get some of the contract dollars previously allotted for PHOs’ administrative costs.
Hospitals also see advantages in contracting directly with health plans. They believe they can negotiate better reimbursement for inpatient care than they can obtain under global capitation, where they need to satisfy the reimbursement demands of the medical staff, often to the detriment of the hospital.
![]() mployers are beginning to take a
more active role in the Indianapolis health care market, not through joint purchasing
but through a collaborative group called the Roundtable, whose objective is to gather
comparative information on health plans. Formed in 1997 by Eli Lilly and several other
major Indianapolis employers, the Roundtable has issued a common request for information
(RFI) to health plans. All but one HMO has agreed to participate. One health plan respondent
suggested that by consolidating employers’ information requests, the Roundtable’s RFI has
already reduced plans’ administrative costs.
mployers are beginning to take a
more active role in the Indianapolis health care market, not through joint purchasing
but through a collaborative group called the Roundtable, whose objective is to gather
comparative information on health plans. Formed in 1997 by Eli Lilly and several other
major Indianapolis employers, the Roundtable has issued a common request for information
(RFI) to health plans. All but one HMO has agreed to participate. One health plan respondent
suggested that by consolidating employers’ information requests, the Roundtable’s RFI has
already reduced plans’ administrative costs.
Roundtable employers also have contracted with a vendor to conduct a health status assessment of selected managed care and fee-for-service employees. In addition, they have made clear their belief that Indianapolis HMOs should achieve accreditation from the National Committee for Quality Assurance (NCQA).
These initiatives represent a significant increase in activity by employers, which in 1996 were a relatively unorganized part of the Indianapolis health care market. Since then, health plan premiums, which had been stable for several years, have started to rise. In 1999, premiums are expected to increase by 6 to 8 percent for large employers and by 10 to 15 percent for small employers. In addition, employers have become increasingly concerned about the ability of health plans to manage care in a way that enhances quality and minimizes consumer complaints.
The Roundtable has brought together Indianapolis’s major employers to address joint concerns regarding their relationships with a relatively diffuse health plan market. The initial focus has been on quality of care, care management and administrative issues. In the future, the Roundtable may serve as a vehicle for supporting care management initiatives such as disease management programs and reporting performance data. And although there are no plans to develop joint purchasing agreements, the Roundtable clearly could serve as a platform for addressing this in the future.
![]() tate policy makers have been
much more active in the health care arena
during the past two years, particularly with respect to managed care. Like many
other states, the Indiana legislature has taken a relatively aggressive position
in enacting new controls over managed care plans, including requirements concerning
grievance resolution, provider access,
the use and distribution of formularies, coverage of new technologies and the annual
submission of standardized
information to the state. In addition, the State Department of Insurance has been
instructed to review data from HMOs annually for NCQA’s Health Plan Employer Data
and Information Set (HEDIS) and release them to the public in a report card format.
tate policy makers have been
much more active in the health care arena
during the past two years, particularly with respect to managed care. Like many
other states, the Indiana legislature has taken a relatively aggressive position
in enacting new controls over managed care plans, including requirements concerning
grievance resolution, provider access,
the use and distribution of formularies, coverage of new technologies and the annual
submission of standardized
information to the state. In addition, the State Department of Insurance has been
instructed to review data from HMOs annually for NCQA’s Health Plan Employer Data
and Information Set (HEDIS) and release them to the public in a report card format.
Respondents suggested several possible explanations for this new legislative posture toward managed care, including a new governor who is more interested in health care issues, the concerns of a small number of influential legislators, the activities of other states and antimanaged care publicity in the national media. It is too early at this time to assess the impact of these new requirements on plans. However, it seems safe to say that health plans in the Indianapolis market will be subject to increasing scrutiny from the public as well as the private sector.
Substantial changes have also been made in Indiana’s Medicaid program, mainly to accommodate the incorporation of the federal Children’s Health Insurance Program (CHIP). Respondents reported that initial enrollment in CHIP, which began in June 1998, has been disappointing. Consequently, the state plans to expand its outreach and enrollment efforts.
![]() he Health and Hospital Corporation
(HHC) of Marion County remains the dominant provider of health services
for the indigent in Indianapolis. Its
flagship facility, Wishard Hospital,
enjoys strong community support
and receives $50 million annually from real estate tax levies; it also benefits
from disproportionate share funding. During the past few years, Wishard
has expanded its capacity to provide
indigent services, launched an innovative managed care program for the uninsured and
renovated and modernized its
physical plant.
he Health and Hospital Corporation
(HHC) of Marion County remains the dominant provider of health services
for the indigent in Indianapolis. Its
flagship facility, Wishard Hospital,
enjoys strong community support
and receives $50 million annually from real estate tax levies; it also benefits
from disproportionate share funding. During the past few years, Wishard
has expanded its capacity to provide
indigent services, launched an innovative managed care program for the uninsured and
renovated and modernized its
physical plant.
In response to growing demands for outpatient care, Wishard has opened three new community health centers since 1996. The number of visits to these centers has increased significantly during the past two years, even though the number of uninsured in Indianapolis has remained relatively constant. The Indiana University Medical Group-Primary Care, a physician group sponsored by HHC and the University’s medical school, runs the centers. In 1997, Wishard launched the Wishard Advantage managed care program for the uninsured, with a benefit package similar to that offered by Indiana’s managed care Medicaid program. Physician services are provided by the University’s primary and specialty care medical groups, and Wishard provides ancillary and inpatient services. Uninsured Marion County residents and their families who are at or below 200 percent of the federal poverty level are eligible. Enrollees with incomes of less than 150 percent of poverty receive free care; others pay a monthly fee on a sliding-scale basis. In the program’s first 18 months, inpatient use reportedly dropped from 800 to 400 days per thousand annually, and emergency room use fell by 30 percent. As of October 1998, Wishard Advantage had 18,800 enrollees.
Because of Wishard’s close ties with the University’s medical school and faculty, officials at Wishard were concerned that the creation of Clarian Health Partners would have a negative impact on their operations and on their relations with medical school faculty. To date, this has not happened. Instead, the merger between Methodist and the University Medical Center has forced Wishard to re-evaluate its relationships with physician groups and the medical school and to consider other options for aligning with physicians. It also has led Wishard to explore alternative relationships with other organizations and to develop new strategies and programs.
![]() uring the past two years, large
provider systems in Indianapolis have remained strong, and some have even expanded
their influence outside the city. The
physician market is consolidating, as physicians try to enhance their negotiating
power with health plans, but at a measured pace. Since 1996, policy
makers have become more active in
the health care arena, particularly concerning managed care. Meanwhile, large
private purchasers have begun to work
collaboratively to influence health plan performance.
uring the past two years, large
provider systems in Indianapolis have remained strong, and some have even expanded
their influence outside the city. The
physician market is consolidating, as physicians try to enhance their negotiating
power with health plans, but at a measured pace. Since 1996, policy
makers have become more active in
the health care arena, particularly concerning managed care. Meanwhile, large
private purchasers have begun to work
collaboratively to influence health plan performance.
As market developments continue to unfold, several issues will be important to track, including the following:
Indianapolis, the highest and lowest HSC study sites and metropolitan areas with over 200,000 population

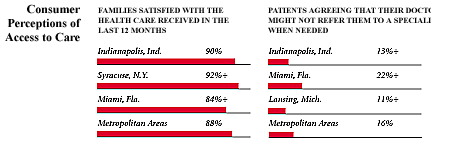


+ Site value is significantly different from the mean for metropolitan
areas over 200,000 population.
The information in these graphs comes from the Household, Physician and Employer
Surveys conducted in 1996 and 1997 as part of HSC’s Community Tracking Study. The
margins of error depend on the community and survey question and include +/- 2
percent to +/- 5 percent for the Household Survey, +/-3 percent to +/-9 percent
for the Physician Survey and +/-4 percent to +/-8 percent for the Employer Survey.
| Indianapolis, Ind. | Metropolitan areas above 200,000 population |
| Population, 19971 | |
| 1,503,468 | |
| Population Change, 1990-19971 | |
| 8.5% | 6.7% |
| Median Income2 | |
| $29,851 | $26,646 |
| Persons Living in Poverty2 | |
| 10% | 15% |
| Persons Age 65 or Older2 | |
| 12% | 12% |
| Persons with No Health Insurance2 | |
| 11% | 14% |
|
Sources: 1. U.S. Census, 1997 2. Household Survey Community Tracking Study, 1996-1997 | |

The Community Tracking Study, the major effort of HSC, tracks changes in the health system in 60 sites that are representative of the nation. Every two years, HSC conducts surveys in all 60 communities and site visits in the following 12 communities: