
Integration Strategies Unravel, Competition Intensifies:
Seattle, Washington
Community Report No. 06
Winter 1999
Douglas L. Fountain, Effie Gournis, Cara S. Lesser, Deborah Alvarez
![]() n 1996, Seattle’s once isolated and
remarkably stable health care market appeared headed for transformation. The prior
few years had witnessed the passage and then repeal of comprehensive state health
reform; Seattle’s largest employer, the Boeing Company, began converting to managed
care; and health plans began contracting selectively with physicians. National
plans eyed the market with new interest, local plans consolidated and took on a
regional focus, while local health systems pursued vertical integration to compete
for managed care business.
n 1996, Seattle’s once isolated and
remarkably stable health care market appeared headed for transformation. The prior
few years had witnessed the passage and then repeal of comprehensive state health
reform; Seattle’s largest employer, the Boeing Company, began converting to managed
care; and health plans began contracting selectively with physicians. National
plans eyed the market with new interest, local plans consolidated and took on a
regional focus, while local health systems pursued vertical integration to compete
for managed care business.
Since 1996, health maintenance organization (HMO) enrollment has not grown as quickly as expected, and several notable changes have occurred:
- Several providers abandoned efforts to operate
their own health plans and revamped their physician integration strategies.
- The local nature of the health plan market appears to be eroding, as plans
increasingly take on a national and regional focus.
- Competition among hospitals has intensified, with a new focus on developing
specialty product lines.
- Turmoil in the individual insurance market and programs for the poor has left fewer plans serving these populations.
- Managed Care Growth Falls Short
- Provider-Sponsored Plans Discontinued
- Providers Reassess Physician Integration Strategies
- Plan Market Increasingly Takes a National and Regional Focus
- Insurance Products for Individuals and the Poor Are in Jeopardy
- Provider Competition Intensifies Along Specialty Lines
- Issues to Track
- Seattle Compared to Other Communities HSC Tracks
- Background and Observations
Managed Care Growth Falls Short
![]() MO enrollment and capitated
payment arrangements have grown more slowly than expected in Seattle, taking
providers and health plans by surprise. Although market penetration by HMOs
rose from 19 percent in January 1996 to 29 percent in July 1997, it still
remains below the average for large metropolitan areas
and low for the West Coast. Meanwhile, providers estimate that capitation
currently accounts for only 25 to 30
percent of their business, far less than they predicted. The popularity of
point-of-service (POS) products in Seattle, as in other communities, may
account for this in part, since capitation
is more difficult to implement under these arrangements.
MO enrollment and capitated
payment arrangements have grown more slowly than expected in Seattle, taking
providers and health plans by surprise. Although market penetration by HMOs
rose from 19 percent in January 1996 to 29 percent in July 1997, it still
remains below the average for large metropolitan areas
and low for the West Coast. Meanwhile, providers estimate that capitation
currently accounts for only 25 to 30
percent of their business, far less than they predicted. The popularity of
point-of-service (POS) products in Seattle, as in other communities, may
account for this in part, since capitation
is more difficult to implement under these arrangements.
Several factors account for the relatively low HMO penetration. Until recently, Seattle’s health care market was made up almost entirely of local not-for-profit health insurers and providers that have coexisted for more than 50 years. Purchasers and consumers have been satisfied with local prices, access and quality. Only the home-grown health plan, Group Health Cooperative of Puget Sound, had substantial HMO enrollment, and this still accounted for a relatively small portion of the overall market. Otherwise, purchasers and consumers favored traditional coverage and preferred provider organizations (PPOs). Because local health care costs and utilization were already low, HMOs had little to offer purchasers in the way of substantial savings, and Seattle’s consumers generally have not been amenable to the constraints of closed-panel HMOs.
Despite this satisfaction with the status quo, dramatic growth in HMO enrollment was expected in the mid-1990s in response to new, far-reaching state policy and purchasing initiatives. In 1993, the state passed a comprehensive health reform bill that mandated health insurance coverage and was expected to drive most of the state’s population into HMOs. However, major provisions of the act were repealed between 1994 and 1996, thus preventing this from occurring. Although the state moved forward with HMO enrollment for public employees, Medicaid beneficiaries and those in the state-sponsored health insurance program, the Basic Health Plan (BHP), there was no broad-scale conversion of the commercially insured from PPOs and indemnity coverage as had been expected.
Another anticipated driver of HMO enrollment growth came in 1996, when Boeing began providing incentives for employees to enroll in managed care products - a move expected to lead other purchasers in the same direction. Although Boeing successfully increased enrollment in HMOs from 10 to 50 percent of its work force, other employers have yet to follow suit, and the overall impact on the market has been more modest than expected.
Provider-Sponsored Plans Discontinued
![]() n light of changing market conditions,
a number of providers have abandoned efforts to operate their own health plans, due in part to administrative challenges and lower-than-expected returns on investment. Two of the major provider systems in Seattle - Providence Health System and Virginia Mason Medical Center - sold off their large plans. The Providence plan was sold to the local Blue Shield plan, Regence Blue Shield, and Virginia Mason’s plan was sold to Aetna U.S. Healthcare, facilitating Aetna’s return to the market. In addition, a
health plan established by the state medical society in 1995, Unified Physicians of Washington, closed its doors after sustaining large losses.
Finally, Care Net, a plan sponsored by the University of Washington and
Premera Blue Cross, was eliminated when Premera consolidated it with other products.
n light of changing market conditions,
a number of providers have abandoned efforts to operate their own health plans, due in part to administrative challenges and lower-than-expected returns on investment. Two of the major provider systems in Seattle - Providence Health System and Virginia Mason Medical Center - sold off their large plans. The Providence plan was sold to the local Blue Shield plan, Regence Blue Shield, and Virginia Mason’s plan was sold to Aetna U.S. Healthcare, facilitating Aetna’s return to the market. In addition, a
health plan established by the state medical society in 1995, Unified Physicians of Washington, closed its doors after sustaining large losses.
Finally, Care Net, a plan sponsored by the University of Washington and
Premera Blue Cross, was eliminated when Premera consolidated it with other products.
While slow HMO enrollment prevented these provider-sponsored plans from achieving the scale they needed to be viable, they faced additional problems. Most of the plans were created to support the provider’s primary business lines by acting as a referral feeder and increasing the provider’s name recognition and geographic reach. But the administrative challenges of operating a plan diverted management’s attention and resources from the core business.
Plan growth also was complicated by the fact that no single provider system possessed sufficient geographic coverage on its own to serve the broader Puget Sound area, much less the entire state, and securing favorable contracts with hospitals or physicians in outlying areas was difficult. Outside of downtown Seattle, plans frequently found few potential contracting partners, making it hard for them to obtain price concessions or influence care management.
Providers Reassess Physician Integration Strategies
![]() he lackluster managed care environment - along with an oversupply of physicians and low prices paid for
services - also has contributed to Seattle providers’ re-evaluation of the ownership-based physician integration strategies they had been pursuing for several years. For example, Virginia Mason, a multi-specialty physician group with clinics throughout northwestern Washington and a hospital in Seattle, had pursued growth through acquisition of additional practices. However, limited returns on these investments and the demand for broad physician networks led the group to shift its focus to developing contractual relationships rather than purchasing additional groups.
he lackluster managed care environment - along with an oversupply of physicians and low prices paid for
services - also has contributed to Seattle providers’ re-evaluation of the ownership-based physician integration strategies they had been pursuing for several years. For example, Virginia Mason, a multi-specialty physician group with clinics throughout northwestern Washington and a hospital in Seattle, had pursued growth through acquisition of additional practices. However, limited returns on these investments and the demand for broad physician networks led the group to shift its focus to developing contractual relationships rather than purchasing additional groups.
Perhaps the most striking development has been at Medalia Healthcare, Puget Sound’s largest primary care group. Medalia was launched in 1994 by Providence Health System in Seattle and Franciscan Health System in neighboring Tacoma. Amassing 45 clinics and more than 300 physicians, the group quickly gained favor in the market and secured an important contract with Providence’s health plan for Boeing employees. However, Medalia counted on large-scale capitated enrollment to cover costs, a feat it was unable to achieve in a market that remains dominated by PPOs. The group’s original business plan projected it would have four times the number of capitated lives by 1998 than it currently manages.
The pressures on Medalia came to a head in late 1998, when it announced a major reorganization. Medalia was divided into three geographic-focused operating units, reduced its number of clinics and established tighter relationships with specialists and affiliated hospitals. In Seattle, it signed contracts with the market’s two largest multispecialty groups, PolyClinic and Minor and James, which give Medalia preferential rates, risk sharing for capitated lives and a stronger referral base - all of which is expected to help stabilize its position. While the effectiveness of this strategy remains to be seen, it is illustrative of the ways in which Seattle providers are now moving to adapt to the unexpected slow growth of capitation.
Plan Market Increasingly Takes a National and Regional Focus
![]() ntil a few years ago, Seattle
was served primarily by a handful of local health plans, with 70 to 75 percent of
the market enrolled in one of three local plans. By 1996, however, two national
health plans had entered the Seattle marketplace, and since then three more have
come in,
gaining some market share from the
three dominant local plans.
ntil a few years ago, Seattle
was served primarily by a handful of local health plans, with 70 to 75 percent of
the market enrolled in one of three local plans. By 1996, however, two national
health plans had entered the Seattle marketplace, and since then three more have
come in,
gaining some market share from the
three dominant local plans.
Because costs and utilization have historically been low in Seattle, it was seen as a market that outside plans would find difficult to enter. In fact, recent entrants have come into Seattle through acquisition or affiliation.
- Kaiser Permanente Northwest affiliated with Seattle’s largest HMO, Group Health.
- Aetna U.S. Healthcare acquired Virginia Mason’s health plan and, through its
national acquisition, NYLCare’s local enrollees.
- United HealthCare entered through its national acquisition of Travelers’ small number of local enrollees.
Meanwhile, the two local Blues’ plans continued to expand beyond Seattle, to the broader regional area. Blue Cross of Washington and Alaska, renamed Premera Blue Cross, has been marketing throughout the northwest, and many of the Blue Shield plans that had operated independently in each county in Washington and surrounding states consolidated to form Regence Blue Shield.
The emerging national and regional focus in the health plan market appears to be in response to the way the Seattle economy is developing. Boeing’s recent merger with McDonnell Douglas has given the local employer a new national perspective, prompting it to standardize its employee benefits nationwide. Similarly, other mergers of local companies with national corporations-including Seattle-based SeaFirst Bank with BankAmerica and Northwest-based grocery chain Fred Meyer with Kroger-appear to be pushing more employers to seek contracts that serve a broad regional and national employee base.
The influx of national plans has pushed local organizations to respond to new products and changing market conditions. For example, PacifiCare’s entrance prior to 1996 severely challenged Group Health’s Medicare market share by introducing a zero premium product. Group Health responded with its own zero premium product, which strained it financially. Group Health looked to its 1996 affiliation with Kaiser to help protect its position, but the impact of this affiliation remains unclear, and it is now reportedly scaling back on this relationship. At the time of the affiliation, it was thought that Kaiser would provide Group Health access to national accounts and provide the resources needed to improve its information infrastructure, facilities and overall competitiveness. However, some observers now question whether the anticipated changes will ever take place. While Group Health still accounts for the largest share of Seattle’s HMO enrollment, it continues to lose market share and endure financial losses as it struggles with changing market conditions.
Insurance Products for Individuals and the Poor Are in Jeopardy
![]() ealth plans in Seattle, as in other
markets, have experienced significant financial losses in recent years, and they
have been especially hard-hit locally by problems with products in the individual
market and public insurance programs.
ealth plans in Seattle, as in other
markets, have experienced significant financial losses in recent years, and they
have been especially hard-hit locally by problems with products in the individual
market and public insurance programs.
In the individual market, insurance reforms, including portability, guaranteed issue, limits on pre-existing condition prohibitions and mandated benefits, have increased plans’ costs. Meanwhile, the state has placed limits on plans’ ability to increase their premiums. In 1996, Premera Blue Cross-the largest individual insurance carrier-sued for a 19 percent rate increase that bypassed state limits. Although it secured the increase, continued losses led Premera to announce that it would stop accepting applications for individual policies in December 1998. Seattle’s other individual carriers, Group Health and Regence Blue Shield, have also sought regulatory approval to cap enrollment on certain individual products. Some carriers also have scaled back the benefits offered under these products, making them less attractive to those with higher health care needs.
Many individuals now appear to be turning to the state’s BHP, which provides subsidized coverage for the working poor and extends nonsubsidized coverage to individuals at higher income levels. Because BHP benefits are more comprehensive than many individual policies, the nonsubsidized component of the program has experienced adverse selection. One of the most visible ways in which this has been manifested is in enrollment for maternity care. BHP is one of the few individual products in the market that offers immediate coverage of obstetrical and newborn care. This has become problematic for the program because pregnant women have been enrolling for this coverage and then dropping out of BHP after they deliver.
At the same time, the program has been beset by adverse selection-resulting from an influx of beneficiaries from the state’s high-risk pool closed to new enrollees in 1996 subsequent to insurance reforms. Excluding maternity-related care, inpatient utilization rates for nonsubsidized BHP enrollees are nearly two and a half times higher than those of subsidized enrollees. Soaring costs have led BHP rates for nonsubsidized enrollees to increase by 62 percent from 1998 to 1999, following a similar increase from 1997 to 1998. By contrast, BHP rates for subsidized enrollees rose by only 9 percent.
Seattle’s health plans also have had problems with the state’s Medicaid program, Healthy Options, particularly with automatic enrollees-beneficiaries who have not selected a plan and who are assigned to one based on a formula. The lowest-cost plan receives 60 percent of auto-enrollees, the next lowest-cost plan gets 30 percent and the remaining 10 percent are enrolled with the next lowest-cost plan. Health plan respondents note that, as a group, auto-enrollees have higher than average health costs, which were not included in their original rate bids. As a result, several plans are pricing their products higher to avoid auto-enrollees; other plans have withdrawn from Healthy Options altogether. In Seattle, Providence reportedly had the lowest-cost plan until it dropped out of Healthy Options, leaving QualMed as the lowest-cost plan until it also pulled out. Elsewhere in the state, Premera Blue Cross and other large plans have pulled out of Healthy Options.
Plans’ difficulties in Healthy Options and BHP are compounded by the state’s joint procurement process for these products. The state requires plans to offer both products if they wish to offer either. Consequently, the decision to discontinue one of these products has meant that the plan drops out of both, although some exceptions have been made recently.
Provider and health plan representatives and advocates for the poor believe that many of the challenges faced by the individual market, the Healthy Options program and the nonsubsidized BHP could be addressed by technical solutions. Indeed, the state is currently debating options such as an enrollment lock-in for the BHP, risk-adjusted rates or incentives for continuous coverage that may help to alleviate some of these problems. In the meantime, respondents have expressed concern that the problems in these markets and the concurrent plan withdrawals are increasingly constraining choice for consumers, particularly the poor.
Provider Competition Intensifies Along Specialty Lines
![]() ew pressures are confronting
Seattle providers as recent alliances cause
referrals to be redirected and as
health plans squeeze reimbursement. Competition has intensified among area
hospitals around key specialty lines,
such as cardiac and cancer care. As a result, a more aggressive dynamic has
emerged, and hospitals that were once praised for fostering a cooperative
culture and serving community interests are
now seen as seeking to enhance their
reputation and market position at the expense of other hospitals.
ew pressures are confronting
Seattle providers as recent alliances cause
referrals to be redirected and as
health plans squeeze reimbursement. Competition has intensified among area
hospitals around key specialty lines,
such as cardiac and cancer care. As a result, a more aggressive dynamic has
emerged, and hospitals that were once praised for fostering a cooperative
culture and serving community interests are
now seen as seeking to enhance their
reputation and market position at the expense of other hospitals.
Competition in cardiac care escalated in 1996 when Group Health established a jointly sponsored point-of-service product with Virginia Mason and closed its downtown hospital. As a result, tertiary care, including high-end cardiac care that had previously gone to the University of Washington, was shifted to Virginia Mason. The University of Washington sought to make up for the volume it lost by undertaking a cardiac-care joint venture with Northwest Hospital. Meanwhile, Swedish Medical Center wrested the majority of cardiologists from Providence Seattle Medical Center and established a new cardiac health management program to aggressively pursue this business.
Similar competition has emerged in cancer care services. Fred Hutchinson Cancer Research Center is launching the Cancer Care Alliance with the University of Washington and Children’s Hospital. The alliance includes a jointly sponsored outpatient center and an arrangement to direct inpatient care exclusively to the University of Washington Medical Center and Children’s Hospital. Previously, Fred Hutchinson referred inpatient care to Swedish Medical Center or Children’s; now Swedish reportedly stands to lose about 9 percent of its daily census. New competition for cancer care also has come into the market, with the entry of national carve-out specialty management companies, such as Cancer Treatment Centers of America.
These changes represent a return to competition in core lines of business at a time when vertical integration strategies seem less assured of success and positioning for capitated contracting has become less of a focus. Under mounting cost pressure, hospitals have looked to secure key specialty lines to lock in referrals and income from this business. The new competitive dynamic that has consequently emerged marks a shift in how Seattle providers operate. Indeed, some respondents speculated about whether this competitive behavior can be sustained or will lead to some consolidation of tertiary hospitals or services in the future.
Issues to Track
![]() scalating competition and
the entrance of several national actors in the Seattle market have prompted
local organizations to find ways to protect and enhance their core businesses.
As managed care growth plateaus, providers, health plans and state policy makers
appear to be in the midst of a period of reassessment
and adaptation. Several trends are worth tracking in this regard:
scalating competition and
the entrance of several national actors in the Seattle market have prompted
local organizations to find ways to protect and enhance their core businesses.
As managed care growth plateaus, providers, health plans and state policy makers
appear to be in the midst of a period of reassessment
and adaptation. Several trends are worth tracking in this regard:
- What new strategies will emerge as providers move away from vertical
integration? Will a new emphasis on exclusivity via contractual arrangements and
joint ventures take its place?
- How will intensifying competition along specialty lines affect relationships
among physicians, hospitals and plans? Will the aggressive pursuit of this
business lead to some consolidation
of tertiary care in the market?
- Will the local nature of the Seattle
market continue to erode, given the growing role of national plans and ongoing
efforts by local plans to
regionalize?
- What impact will emerging difficulties in individual insurance markets, the Medicaid Healthy Options program and BHP have on health plans and beneficiaries? Will state policy interventions succeed in addressing these problems?
Seattle Compared to Other Communities HSC Tracks
Seattle, the highest and lowest HSC study sites and metropolitan areas with over 200,000 population

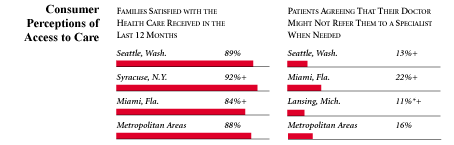

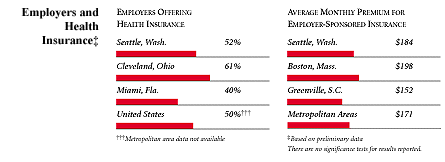
+Site value is significantly different from the mean for metropolitan areas over 200,000
population.
The information in these graphs comes from the Household, Physician and Employer
Surveys conducted in 1996 and 1997 as part of HSC’s Community Tracking Study. The
margins of error depend on the community and survey question and include +/- 2
percent to +/- 5 percent for the Household Survey, +/-3 percent to +/-9 percent
for the Physician Survey and +/-4 percent to +/-8 percent for the Employer Survey.
Background and Observations
Seattle Demographics
| Seattle, Wash. | Metropolitan areas above 200,000 population |
| Population, 19971 | |
| 2,268,126 | |
| Population Change, 1990-19971 | |
| 11% | 6.7% |
| Median Income2 | |
| $31,561 | $26,646 |
| Persons Living in Poverty2 | |
| 8.1% | 15% |
| Persons Age 65 or Older2 | |
| 12% | 12% |
| Persons with No Health Insurance2 | |
| 8.3% | 14% |
|
Sources: 1. U.S. Census, 1997 2. Household Survey Community Tracking Study, 1996-1997 | |

The Community Tracking Study, the major effort of HSC, tracks changes in the health system in 60 sites that are representative of the nation. Every two years, HSC conducts surveys in all 60 communities and site visits in the following 12 communities:
- Boston, Mass.
- Cleveland, Ohio
- Greenville, S.C.
- Indianapolis, Ind.
- Lansing, Mich.
- Little Rock, Ark.
- Miami, Fla.
- Newark, N.J.
- Orange County, Calif.
- Phoenix, Ariz.
- Seattle, Wash.
- Syracuse, N.Y.